Sun, Apr 5, 2026
[Archive]
Volume 23, Issue 9 (September 2025)
IJRM 2025, 23(9): 749-758 |
Back to browse issues page
Ethics code: IR.MUMS.MEDICAL.REC.1400.001
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Hatamian Z, Mousavi Vahed S H, Vakilian F, Poorzand H, Lotfalizade M, Zirak N, et al . N-terminal pro-B-type natriuretic peptide levels in pregnant women with heart disease and complications: A cohort study. IJRM 2025; 23 (9) :749-758
URL: http://ijrm.ir/article-1-3152-en.html
URL: http://ijrm.ir/article-1-3152-en.html
Zahra Hatamian1 

 , Seyede Houra Mousavi Vahed *2
, Seyede Houra Mousavi Vahed *2 

 , Farveh Vakilian3
, Farveh Vakilian3 

 , Hoorak Poorzand4
, Hoorak Poorzand4 

 , Marzieh Lotfalizade1
, Marzieh Lotfalizade1 

 , Nahid Zirak5
, Nahid Zirak5 

 , Hassan Mehrad Majd6
, Hassan Mehrad Majd6 

 , Marzieh Nozari7
, Marzieh Nozari7 

 , Salmeh Dadgar1
, Salmeh Dadgar1 

 , Malihe Afiat1
, Malihe Afiat1 




 , Seyede Houra Mousavi Vahed *2
, Seyede Houra Mousavi Vahed *2 

 , Farveh Vakilian3
, Farveh Vakilian3 

 , Hoorak Poorzand4
, Hoorak Poorzand4 

 , Marzieh Lotfalizade1
, Marzieh Lotfalizade1 

 , Nahid Zirak5
, Nahid Zirak5 

 , Hassan Mehrad Majd6
, Hassan Mehrad Majd6 

 , Marzieh Nozari7
, Marzieh Nozari7 

 , Salmeh Dadgar1
, Salmeh Dadgar1 

 , Malihe Afiat1
, Malihe Afiat1 


1- Department of Obstetrics and Gynecology, Faculty of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran.
2- Department of Obstetrics and Gynecology, Faculty of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran. ,vahedalainh@mums.ac.ir
3- Department of Cardiology, Faculty of Medicine, Lung Diseases Research Center, Imam Reza Hospital, Mashhad University of Medical Sciences, Mashhad, Iran.
4- Department of Cardiology, Faculty of Medicine, Vascular and Endovascular Surgery Research Center, Imam Reza Hospital, Mashhad University of Medical Sciences, Mashhad, Iran.
5- Department of Anesthesiology, Faculty of Medicine, Lung Diseases Research Center, Imam Reza Hospital, Mashhad University of Medical Sciences, Mashhad, Iran.
6- Department of Medical Genetics and Molecular Medicine, Faculty of Medicine, Cancer Molecular Pathology Research Center, Mashhad University of Medical Sciences, Mashhad, Iran.
7- Department of Midwifery, Faculty of Nursing and Midwifery, Mashhad University of Medical Sciences, Mashhad, Iran.
2- Department of Obstetrics and Gynecology, Faculty of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran. ,
3- Department of Cardiology, Faculty of Medicine, Lung Diseases Research Center, Imam Reza Hospital, Mashhad University of Medical Sciences, Mashhad, Iran.
4- Department of Cardiology, Faculty of Medicine, Vascular and Endovascular Surgery Research Center, Imam Reza Hospital, Mashhad University of Medical Sciences, Mashhad, Iran.
5- Department of Anesthesiology, Faculty of Medicine, Lung Diseases Research Center, Imam Reza Hospital, Mashhad University of Medical Sciences, Mashhad, Iran.
6- Department of Medical Genetics and Molecular Medicine, Faculty of Medicine, Cancer Molecular Pathology Research Center, Mashhad University of Medical Sciences, Mashhad, Iran.
7- Department of Midwifery, Faculty of Nursing and Midwifery, Mashhad University of Medical Sciences, Mashhad, Iran.
Full-Text [PDF 656 kb]
(449 Downloads)
| Abstract (HTML) (460 Views)
Full-Text: (98 Views)
1. Introduction
Managing pregnant individuals with cardiovascular diseases presents a significant challenge (1). This difficulty arises due to the physiological changes in the cardiovascular system during pregnancy (2). Increased cardiac output and blood volume during this period place additional strain on cardiac reserve, often exacerbating pre-existing cardiovascular conditions. Studies report that up to 4% of pregnancies involve newly diagnosed cardiovascular diseases, which can result in a mortality rate as high as 15% (3).
Cardiovascular disease during pregnancy has been associated with various maternal and neonatal complications. These include excessive weight gain, preterm birth, preeclampsia, intrauterine growth restriction, gestational diabetes, progressive heart failure, placental abruption, and, in severe cases, maternal or fetal death (4).
N-terminal pro-B-type natriuretic peptide (NT-proBNP) is a key biomarker for cardiovascular health. It has a longer half-life and greater diagnostic accuracy than BNP (5, 6). Previous studies have demonstrated its potential for predicting morbidity and mortality in individuals with cardiovascular conditions (7-12). However, its impact on pregnancy outcomes in women with cardiovascular disease remains unclear, necessitating further research (13, 14).
This study aims to examine the relationship between serum levels of NT-proBNP in pregnant women with cardiovascular disease and associated fetomaternal complications.
2. Materials and Methods
2.1. Study design and sample
This cohort study was conducted at the Heart and Pregnancy Clinic of Imam Reza hospital in Mashhad, Iran, from July 2019-July 2020. The study focused on 50 pregnant women with heart disease in their third trimester (from 28 wk onward). Participants were required to have a New York Heart Association (NYHA) classification of class II or higher. Exclusion criteria included an inability or unwillingness to cooperate with researchers, difficulty attending regular check-ups, proximity to delivery, or failure to meet the NYHA class II or higher requirement.
2.2. Data gathering and follow up
The participants' demographic and medical data were collected through interviews and specialized checklists. All subjects underwent echocardiographic evaluation performed by cardiologists at the Heart and Pregnancy Clinic, Imam Reza hospital, Mashhad, Iran and were classified according to the NYHA classification (Figure 1) (15).
After diagnosing heart failure, the severity of the disease was classified based on symptoms using the NYHA classification. It was further categorized into 3 groups based on pulmonary artery pressure and ejection fraction (16). Additionally, all participants underwent a 12-lead ECG to assess whether their cardiac function was normal or abnormal. The study monitored participants for cardiovascular symptoms, including respiratory distress and chest pain, during 3 visits at one-month intervals. Echocardiography was performed twice, with a 2-month gap between assessments. The research also examined the occurrence of various obstetric and pregnancy complications, such as intrauterine growth restriction, hypertension, preterm delivery, emergency cesarean section, the need for maternal hospitalization in specialized care units, and neonatal complications.
Furthermore, the study recorded maternal and neonatal intensive care unit (ICU) admission rates, mode of delivery, persistence of cardiovascular symptoms, continuation of medication, echocardiographic findings, and relevant medical history.
2.3. NT-proBNP assessment
A 0.5 cc blood sample was collected from the brachial vein to measure NT-proBNP levels using a VIDAS kit manufactured in France. Based on these levels, participants were categorized into 2 groups: those with normal NT-proBNP levels (n = 37) and those with elevated NT-proBNP levels (n = 13). The optimal cut-off value for classification was set at 125 pg/mL (17-19). Study data were then compared between participants with normal and elevated NT-proBNP levels.
2.4. Sample size
Based on NT-proBNP serum levels in pregnant women with preexisting heart disease and associated complications during pregnancy and fetal development, changes in NT-proBNP levels were used to determine the required sample size. A specific formula was applied to calculate the population mean.
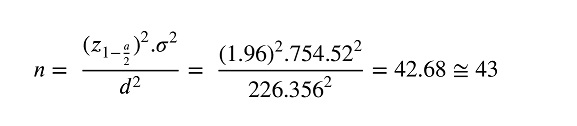
Using a standard deviation of 754.52 (associated with NT-proBNP serum levels) from a previous study (20), a significance level of 0.05, and d = 226.356, the sample size was estimated accordingly.

2.5. Ethical Considerations
The study protocol was approved by the Ethics Committee of Mashhad University of Medical Sciences, Mashhad, Iran (Code: IR.MUMS.MEDICAL.REC.1400.001). The study's objectives and general details were explained to all participants, and written informed consent was obtained before participation.
2.6. Statistical Analysis
The data were entered into SPSS (Statistical Package for the Social Sciences, version 17.0, SPSS Inc., Chicago, Illinois, USA) for analysis. The frequency and percentage of qualitative data were calculated, along with the mean, median, standard deviation, and interquartile range for quantitative data. Qualitative data were compared between the 2 study groups using the Chi-square and Fisher’s exact tests, while quantitative data were analyzed using an independent sample t test. A p < 0.05 was considered statistically significant. Written informed consent was obtained from all participants.
3. Results
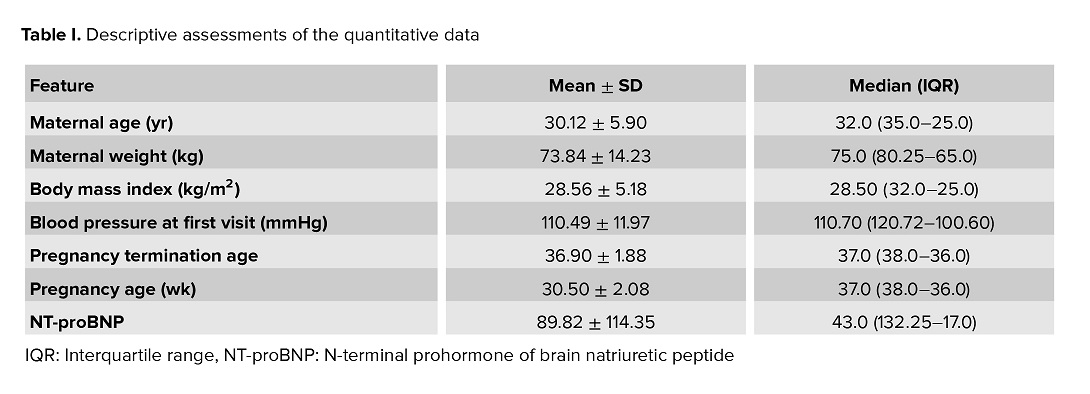
A total of 50 women, with an average age of 30.12 ± 5.90 yr and an average pregnancy age of 30.5 ± 2.08 wk, were included in the study (Table I).
Table II provides a detailed analysis of the qualitative data, demonstrating that at the first visit, only 2 cases (4.0%) were found to have hypertension.
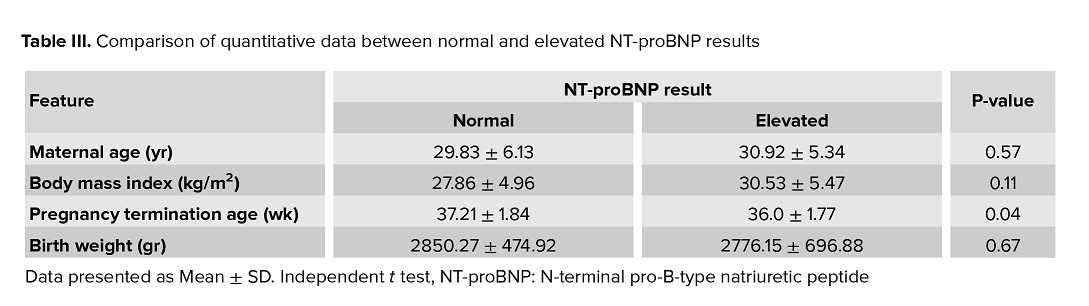
Table III compares maternal age, body mass index, pregnancy termination age, birth weight, and hemoglobin levels between normal and elevated NT-proBNP results. The data clearly shows that the pregnancy termination age was significantly lower in the elevated NT-proBNP group (p = 0.04).
The elevated NT-proBNP group exhibited a higher frequency of low Apgar scores (p = 0.05) and increased blood pressure during both the second (p = 0.05) and third visits (p < 0.0001) (Table IV).
The frequency of elevated NT-proBNP was significantly higher during the second (p = 0.05) and third visits (p < 0.001). Moreover, drug history showed a significant difference between these 2 groups (p < 0.001) (Table IV).



4. Discussion
In our study, we aimed to assess the impact of NT-proBNP on maternal and neonatal outcomes in mothers with cardiovascular diseases. Our findings revealed a significantly higher incidence of hypertension among participants with elevated NT-proBNP levels (using a cut-off of 125 pg/mL). However, we did not find a significant association between NT-proBNP levels and maternal outcomes such as ICU admission, mode of delivery, symptom persistence, or continued medication use. Additionally, no significant differences were observed in ECG and echocardiographic findings between the 2 groups across 2 visits. Nevertheless, our study suggests a potential link between elevated NT-proBNP levels and the development of hypertension during pregnancy. Furthermore, we identified an association between elevated NT-proBNP levels and lower Apgar scores in newborns within our study group.
NT-proBNP is a well-established biomarker commonly used in patients with heart failure (21). Additionally, studies have reported that NT-proBNP can predict major adverse cardiovascular events in pre-diabetic individuals (22). The significant association between elevated NT-proBNP levels and increased cardiovascular and all-cause mortality in a diverse population of elderly patients in primary care highlights its potential as a valuable tool for identifying individuals at high risk for cardiac events, independent of traditional risk factors (23).
It was found that BNP is associated with an increased risk of all-cause mortality and cardiovascular events even in a healthy population (24). Furthermore, a meta-analysis involving 87,747 subjects demonstrated that higher natriuretic peptide levels were linked to a threefold increase in cardiovascular risk (25).
The significance of NT-proBNP levels during pregnancy should not be overlooked. Research has explored its diagnostic potential in conditions such as gestational hypertension, diabetes, and preeclampsia. Studies indicate that individuals with preeclampsia, gestational hypertension, and gestational diabetes have significantly elevated NT-proBNP levels compared to healthy controls (26-28).
Additionally, a study conducted by Siegmund reported a significant association between high NT-proBNP levels and the development of cardiovascular complications in mothers with congenital heart disease (28). However, in our study, we did not find a significant association between NT-proBNP levels and other maternal outcomes. These discrepancies may be attributed to variations in the cut-off values used across different studies. Studies has reported different reference limits for NT-proBNP levels based on sex, age, and population characteristics (29-32).
We evaluated the standard cut-off of 125 pg/mL and found a potential association between elevated NT-proBNP levels (> 125 pg/mL) and the development of gestational hypertension during pregnancy follow ups. Furthermore, different BNP thresholds have been linked to cardiac events in pregnant individuals (32, 33).
A study reported a correlation between NT-proBNP levels and neonatal outcomes, showing that elevated NT-proBNP levels were associated with low Apgar scores and low birth weight. Consistent with their findings, our study also observed a significantly higher frequency of low Apgar scores in participants with elevated NT-proBNP levels (34).
Some of these discrepancies may be attributed to variations in the adopted cut-off values (29). In our study, we used a cut-off of 125 pg/mL, whereas Siegmund et al. suggested a higher threshold of 235 pg/mL (28).
A meta-analysis evaluating NT-proBNP levels highlighted that the number of included studies was limited, and there was inconsistency regarding the optimal cut-off value. Further research is necessary to validate the prospective use of NT-proBNP in assessing common symptoms indicative of cardiac complications during labor. Additionally, more studies are needed to establish the clinical utility of NT-proBNP testing in this context. There is a known association between NT-proBNP levels and blood pressure in pregnant women. However, the optimal cut-off point for predicting complications remains uncertain. A threshold of 125 pg/mL has been linked to increased maternal blood pressure and lower pregnancy termination age. Additionally, NT-proBNP levels have been associated with low birth weight. Further research is required to determine the most accurate prognostic and diagnostic thresholds.
4.1. Strengths and limitations
The study's findings are significant in 2 key areas: expanding current knowledge and guiding future research on NT-proBNP in pregnant women with heart conditions. Additionally, they provide valuable insights for healthcare providers in managing pregnant women with cardiovascular diseases. Further research is needed to establish precise NT-proBNP thresholds for clinical use.
This study was conducted on pregnant women in Iran, which may limit the generalizability of its findings to a broader population. Research on different ethnic groups could reveal subtle variations, emphasizing the importance of studying diverse populations.
Despite this limitation, the study had notable strengths, including its longitudinal and prospective design, with 2 assessments conducted at distinct intervals. This approach helped minimize data gaps and provided comprehensive insights for researchers. Furthermore, given the limited research available in this field, this study bridges a significant gap in literature, highlighting its importance.
5. Conclusion
The study found no significant association between NT-proBNP levels and maternal outcomes such as ICU admission, delivery method, symptom persistence, or medication continuation. However, elevated NT-proBNP levels were linked to hypertension during pregnancy and lower Apgar scores in newborns.
Larger studies with diverse cut-off values in pregnant populations are needed to establish accurate NT-proBNP thresholds. Further research is essential to better understand the implications of NT-proBNP levels in pregnancy and their impact on both maternal and neonatal health. Conducting broader studies across varied populations and cut-off values can help healthcare providers assess the predictive value of NT-proBNP in identifying high-risk pregnancies and implementing appropriate interventions. Understanding the relationship between NT-proBNP levels and pregnancy complications could ultimately improve prenatal care and outcomes.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author Contributions
Z. Hatamian and SH. Mousavi Vahed had full access to all the data in the study and take responsibility for the integrity and accuracy of the data analysis. Concept and design were done by N. Zirak, H. Poorzand, and F. Vakillian. Acquisition, analysis, or interpretation of data were done by H. Mehrad Majd. Drafting of the manuscript: M. Lotfalizadeh, M. Afiat, and M. Nozari. Critical revision of the manuscript for important intellectual content: All authors. Statistical analysis was done by H. Mehrad Majd and S. Dadgar reviewed the article. All authors approved the final manuscript and take responsibility for the integrity of the data.
Acknowledgments
The researchers express their gratitude to the Research and Technology Vice-Chancellor of Mashhad University of Medical Sciences, Mashhad, Iran, for their scientific support. No artificial intelligence was used in the writing of this article.
Conflict of Interest
The authors declare that there is no conflict of interest.
Managing pregnant individuals with cardiovascular diseases presents a significant challenge (1). This difficulty arises due to the physiological changes in the cardiovascular system during pregnancy (2). Increased cardiac output and blood volume during this period place additional strain on cardiac reserve, often exacerbating pre-existing cardiovascular conditions. Studies report that up to 4% of pregnancies involve newly diagnosed cardiovascular diseases, which can result in a mortality rate as high as 15% (3).
Cardiovascular disease during pregnancy has been associated with various maternal and neonatal complications. These include excessive weight gain, preterm birth, preeclampsia, intrauterine growth restriction, gestational diabetes, progressive heart failure, placental abruption, and, in severe cases, maternal or fetal death (4).
N-terminal pro-B-type natriuretic peptide (NT-proBNP) is a key biomarker for cardiovascular health. It has a longer half-life and greater diagnostic accuracy than BNP (5, 6). Previous studies have demonstrated its potential for predicting morbidity and mortality in individuals with cardiovascular conditions (7-12). However, its impact on pregnancy outcomes in women with cardiovascular disease remains unclear, necessitating further research (13, 14).
This study aims to examine the relationship between serum levels of NT-proBNP in pregnant women with cardiovascular disease and associated fetomaternal complications.
2. Materials and Methods
2.1. Study design and sample
This cohort study was conducted at the Heart and Pregnancy Clinic of Imam Reza hospital in Mashhad, Iran, from July 2019-July 2020. The study focused on 50 pregnant women with heart disease in their third trimester (from 28 wk onward). Participants were required to have a New York Heart Association (NYHA) classification of class II or higher. Exclusion criteria included an inability or unwillingness to cooperate with researchers, difficulty attending regular check-ups, proximity to delivery, or failure to meet the NYHA class II or higher requirement.
2.2. Data gathering and follow up
The participants' demographic and medical data were collected through interviews and specialized checklists. All subjects underwent echocardiographic evaluation performed by cardiologists at the Heart and Pregnancy Clinic, Imam Reza hospital, Mashhad, Iran and were classified according to the NYHA classification (Figure 1) (15).
After diagnosing heart failure, the severity of the disease was classified based on symptoms using the NYHA classification. It was further categorized into 3 groups based on pulmonary artery pressure and ejection fraction (16). Additionally, all participants underwent a 12-lead ECG to assess whether their cardiac function was normal or abnormal. The study monitored participants for cardiovascular symptoms, including respiratory distress and chest pain, during 3 visits at one-month intervals. Echocardiography was performed twice, with a 2-month gap between assessments. The research also examined the occurrence of various obstetric and pregnancy complications, such as intrauterine growth restriction, hypertension, preterm delivery, emergency cesarean section, the need for maternal hospitalization in specialized care units, and neonatal complications.
Furthermore, the study recorded maternal and neonatal intensive care unit (ICU) admission rates, mode of delivery, persistence of cardiovascular symptoms, continuation of medication, echocardiographic findings, and relevant medical history.
2.3. NT-proBNP assessment
A 0.5 cc blood sample was collected from the brachial vein to measure NT-proBNP levels using a VIDAS kit manufactured in France. Based on these levels, participants were categorized into 2 groups: those with normal NT-proBNP levels (n = 37) and those with elevated NT-proBNP levels (n = 13). The optimal cut-off value for classification was set at 125 pg/mL (17-19). Study data were then compared between participants with normal and elevated NT-proBNP levels.
2.4. Sample size
Based on NT-proBNP serum levels in pregnant women with preexisting heart disease and associated complications during pregnancy and fetal development, changes in NT-proBNP levels were used to determine the required sample size. A specific formula was applied to calculate the population mean.
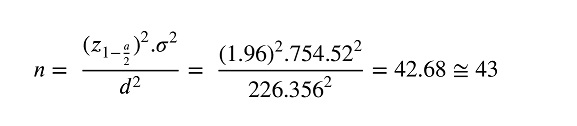
Using a standard deviation of 754.52 (associated with NT-proBNP serum levels) from a previous study (20), a significance level of 0.05, and d = 226.356, the sample size was estimated accordingly.

2.5. Ethical Considerations
The study protocol was approved by the Ethics Committee of Mashhad University of Medical Sciences, Mashhad, Iran (Code: IR.MUMS.MEDICAL.REC.1400.001). The study's objectives and general details were explained to all participants, and written informed consent was obtained before participation.
2.6. Statistical Analysis
The data were entered into SPSS (Statistical Package for the Social Sciences, version 17.0, SPSS Inc., Chicago, Illinois, USA) for analysis. The frequency and percentage of qualitative data were calculated, along with the mean, median, standard deviation, and interquartile range for quantitative data. Qualitative data were compared between the 2 study groups using the Chi-square and Fisher’s exact tests, while quantitative data were analyzed using an independent sample t test. A p < 0.05 was considered statistically significant. Written informed consent was obtained from all participants.
3. Results
A total of 50 women, with an average age of 30.12 ± 5.90 yr and an average pregnancy age of 30.5 ± 2.08 wk, were included in the study (Table I).
Table II provides a detailed analysis of the qualitative data, demonstrating that at the first visit, only 2 cases (4.0%) were found to have hypertension.
Table III compares maternal age, body mass index, pregnancy termination age, birth weight, and hemoglobin levels between normal and elevated NT-proBNP results. The data clearly shows that the pregnancy termination age was significantly lower in the elevated NT-proBNP group (p = 0.04).
The elevated NT-proBNP group exhibited a higher frequency of low Apgar scores (p = 0.05) and increased blood pressure during both the second (p = 0.05) and third visits (p < 0.0001) (Table IV).
The frequency of elevated NT-proBNP was significantly higher during the second (p = 0.05) and third visits (p < 0.001). Moreover, drug history showed a significant difference between these 2 groups (p < 0.001) (Table IV).





4. Discussion
In our study, we aimed to assess the impact of NT-proBNP on maternal and neonatal outcomes in mothers with cardiovascular diseases. Our findings revealed a significantly higher incidence of hypertension among participants with elevated NT-proBNP levels (using a cut-off of 125 pg/mL). However, we did not find a significant association between NT-proBNP levels and maternal outcomes such as ICU admission, mode of delivery, symptom persistence, or continued medication use. Additionally, no significant differences were observed in ECG and echocardiographic findings between the 2 groups across 2 visits. Nevertheless, our study suggests a potential link between elevated NT-proBNP levels and the development of hypertension during pregnancy. Furthermore, we identified an association between elevated NT-proBNP levels and lower Apgar scores in newborns within our study group.
NT-proBNP is a well-established biomarker commonly used in patients with heart failure (21). Additionally, studies have reported that NT-proBNP can predict major adverse cardiovascular events in pre-diabetic individuals (22). The significant association between elevated NT-proBNP levels and increased cardiovascular and all-cause mortality in a diverse population of elderly patients in primary care highlights its potential as a valuable tool for identifying individuals at high risk for cardiac events, independent of traditional risk factors (23).
It was found that BNP is associated with an increased risk of all-cause mortality and cardiovascular events even in a healthy population (24). Furthermore, a meta-analysis involving 87,747 subjects demonstrated that higher natriuretic peptide levels were linked to a threefold increase in cardiovascular risk (25).
The significance of NT-proBNP levels during pregnancy should not be overlooked. Research has explored its diagnostic potential in conditions such as gestational hypertension, diabetes, and preeclampsia. Studies indicate that individuals with preeclampsia, gestational hypertension, and gestational diabetes have significantly elevated NT-proBNP levels compared to healthy controls (26-28).
Additionally, a study conducted by Siegmund reported a significant association between high NT-proBNP levels and the development of cardiovascular complications in mothers with congenital heart disease (28). However, in our study, we did not find a significant association between NT-proBNP levels and other maternal outcomes. These discrepancies may be attributed to variations in the cut-off values used across different studies. Studies has reported different reference limits for NT-proBNP levels based on sex, age, and population characteristics (29-32).
We evaluated the standard cut-off of 125 pg/mL and found a potential association between elevated NT-proBNP levels (> 125 pg/mL) and the development of gestational hypertension during pregnancy follow ups. Furthermore, different BNP thresholds have been linked to cardiac events in pregnant individuals (32, 33).
A study reported a correlation between NT-proBNP levels and neonatal outcomes, showing that elevated NT-proBNP levels were associated with low Apgar scores and low birth weight. Consistent with their findings, our study also observed a significantly higher frequency of low Apgar scores in participants with elevated NT-proBNP levels (34).
Some of these discrepancies may be attributed to variations in the adopted cut-off values (29). In our study, we used a cut-off of 125 pg/mL, whereas Siegmund et al. suggested a higher threshold of 235 pg/mL (28).
A meta-analysis evaluating NT-proBNP levels highlighted that the number of included studies was limited, and there was inconsistency regarding the optimal cut-off value. Further research is necessary to validate the prospective use of NT-proBNP in assessing common symptoms indicative of cardiac complications during labor. Additionally, more studies are needed to establish the clinical utility of NT-proBNP testing in this context. There is a known association between NT-proBNP levels and blood pressure in pregnant women. However, the optimal cut-off point for predicting complications remains uncertain. A threshold of 125 pg/mL has been linked to increased maternal blood pressure and lower pregnancy termination age. Additionally, NT-proBNP levels have been associated with low birth weight. Further research is required to determine the most accurate prognostic and diagnostic thresholds.
4.1. Strengths and limitations
The study's findings are significant in 2 key areas: expanding current knowledge and guiding future research on NT-proBNP in pregnant women with heart conditions. Additionally, they provide valuable insights for healthcare providers in managing pregnant women with cardiovascular diseases. Further research is needed to establish precise NT-proBNP thresholds for clinical use.
This study was conducted on pregnant women in Iran, which may limit the generalizability of its findings to a broader population. Research on different ethnic groups could reveal subtle variations, emphasizing the importance of studying diverse populations.
Despite this limitation, the study had notable strengths, including its longitudinal and prospective design, with 2 assessments conducted at distinct intervals. This approach helped minimize data gaps and provided comprehensive insights for researchers. Furthermore, given the limited research available in this field, this study bridges a significant gap in literature, highlighting its importance.
5. Conclusion
The study found no significant association between NT-proBNP levels and maternal outcomes such as ICU admission, delivery method, symptom persistence, or medication continuation. However, elevated NT-proBNP levels were linked to hypertension during pregnancy and lower Apgar scores in newborns.
Larger studies with diverse cut-off values in pregnant populations are needed to establish accurate NT-proBNP thresholds. Further research is essential to better understand the implications of NT-proBNP levels in pregnancy and their impact on both maternal and neonatal health. Conducting broader studies across varied populations and cut-off values can help healthcare providers assess the predictive value of NT-proBNP in identifying high-risk pregnancies and implementing appropriate interventions. Understanding the relationship between NT-proBNP levels and pregnancy complications could ultimately improve prenatal care and outcomes.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author Contributions
Z. Hatamian and SH. Mousavi Vahed had full access to all the data in the study and take responsibility for the integrity and accuracy of the data analysis. Concept and design were done by N. Zirak, H. Poorzand, and F. Vakillian. Acquisition, analysis, or interpretation of data were done by H. Mehrad Majd. Drafting of the manuscript: M. Lotfalizadeh, M. Afiat, and M. Nozari. Critical revision of the manuscript for important intellectual content: All authors. Statistical analysis was done by H. Mehrad Majd and S. Dadgar reviewed the article. All authors approved the final manuscript and take responsibility for the integrity of the data.
Acknowledgments
The researchers express their gratitude to the Research and Technology Vice-Chancellor of Mashhad University of Medical Sciences, Mashhad, Iran, for their scientific support. No artificial intelligence was used in the writing of this article.
Conflict of Interest
The authors declare that there is no conflict of interest.
Type of Study: Original Article |
Subject:
Pregnancy Health
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |




