Sat, May 30, 2026
[Archive]
Volume 23, Issue 9 (September 2025)
IJRM 2025, 23(9): 739-748 |
Back to browse issues page
Ethics code: IR.MODARES.REC.1397.211
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Azarbayjani K, Jahanian Sadatmahalleh S, Mirzaei N, Yarjanly M, Jahangiri N, Nasiri M et al . Comparison of sexual function in fertile and infertile women with polycystic ovary syndrome: A cross-sectional study. IJRM 2025; 23 (9) :739-748
URL: http://ijrm.ir/article-1-3434-en.html
URL: http://ijrm.ir/article-1-3434-en.html
Khadijeh Azarbayjani1 

 , Shahideh Jahanian Sadatmahalleh *2
, Shahideh Jahanian Sadatmahalleh *2 

 , Negin Mirzaei3
, Negin Mirzaei3 

 , Mahsa Yarjanly1
, Mahsa Yarjanly1 

 , Nadia Jahangiri4
, Nadia Jahangiri4 

 , Malihe Nasiri5
, Malihe Nasiri5 

 , Mona Zeinaloo6
, Mona Zeinaloo6 




 , Shahideh Jahanian Sadatmahalleh *2
, Shahideh Jahanian Sadatmahalleh *2 

 , Negin Mirzaei3
, Negin Mirzaei3 

 , Mahsa Yarjanly1
, Mahsa Yarjanly1 

 , Nadia Jahangiri4
, Nadia Jahangiri4 

 , Malihe Nasiri5
, Malihe Nasiri5 

 , Mona Zeinaloo6
, Mona Zeinaloo6 


1- Department of Reproductive Health and Midwifery, Faculty of Medical Sciences, Tarbiat Modares University, Tehran, Iran.
2- Department of Reproductive Health and Midwifery, Faculty of Medical Sciences, Tarbiat Modares University, Tehran, Iran. ,Shahideh.Jahanian@modares.ac.ir
3- Robinson Research Institute, Faculty of Health and Medical Sciences, University of Adelaide, Adelaide, South Australia.
4- Department of Endocrinology and Female Infertility, Reproductive Biomedicine Research Center, Royan Institute for Reproductive Biomedicine, ACECR, Tehran, Iran.
5- Department of Basic Sciences, Faculty of Nursing and Midwifery, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
6- Department of Community and Preventive Medicine, Faculty of Medicine, Tehran University of Medical Sciences, Tehran, Iran.
2- Department of Reproductive Health and Midwifery, Faculty of Medical Sciences, Tarbiat Modares University, Tehran, Iran. ,
3- Robinson Research Institute, Faculty of Health and Medical Sciences, University of Adelaide, Adelaide, South Australia.
4- Department of Endocrinology and Female Infertility, Reproductive Biomedicine Research Center, Royan Institute for Reproductive Biomedicine, ACECR, Tehran, Iran.
5- Department of Basic Sciences, Faculty of Nursing and Midwifery, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
6- Department of Community and Preventive Medicine, Faculty of Medicine, Tehran University of Medical Sciences, Tehran, Iran.
Keywords: Polycystic ovary syndrome, Infertility, Female sexual function, Reproductive health, Female sexual function index.
Full-Text [PDF 425 kb]
(550 Downloads)
| Abstract (HTML) (709 Views)
Full-Text: (173 Views)
1. Introduction
Polycystic ovarian syndrome (PCOS) is a complex endocrine disorder that affects approximately 9.2% of women of reproductive age globally (1). Ovulatory dysfunction and hyperandrogenism, which includes hirsutism, acne, obesity, and polycystic ovarian morphology, are characteristic of this condition (2).
Furthermore, infertility is defined as the inability to conceive after 1 yr of regular intercourse without contraception, which affects 70-80% of women with PCOS (3). Infertility is a risk factor for sexual dysfunction, as 5-55% of infertile women experience it (4). Infertility not only has a devastating effect on patients' self-esteem but also imposes a lot of financial and psychological burdens on them, consequently, infertility may affect couples' relationships and their satisfaction with sexual intercourse (5). It seems that PCOS is associated with an increased risk of sexual dysfunction as follows: aesthetic factors such as hirsutism, acne, and obesity change the women’s attitude toward their bodies, leading to diminished feminine identity. Imbalance in hormonal profile, hyperandrogenism, and hyperinsulinemia can lead to depression and anxiety that have manifold effects on quality of life (QoL), mental health, and consequently change women’s sexual function (6).
Although in many studies, it is proven that infertility is strongly related to impaired sexual dysfunction, data on the association between sexual function and PCOS are limited and often contradicting (7-10). Thus, in light of previous studies on the detrimental effects of infertility and PCOS on sexual function and the synergistic effects that infertility and PCOS have on each other, infertile PCOS patients might suffer from sexual dysfunction markedly as a comorbidity.
Given the higher prevalence of infertility in women with PCOS, the present study aimed to investigate and compare sexual function as one of the important aspects of women’s lives. The results of the present study, by examining the effects of infertility on women's sexual function, can be used as part of counseling and treatment measures for these patients to reduce the complications of the disease in women with PCOS.
A previous version of this manuscript was presented as a preprint on ResearchSquare prior to peer review. The current version has been revised based on feedback from the peer-review process.
2. Materials and Methods
In this cross-sectional study, 603 women with PCOS who were referred to the Arash hospital gynecological clinics affiliated with Tehran University of Medical Sciences, Tehran, Iran between April 2019 and February 2020 were enrolled through a convenience sampling method. They were categorized into 2 groups: fertile (n = 364) and infertile (n = 239).
Inclusion criteria: married women diagnosed with PCOS based on the Rotterdam criteria (11), aged 18-45 yr, and sexually active in the past 4 wk. Infertility was defined as the inability to conceive after 12 months or more of regular unprotected intercourse, including both primary and secondary infertility.
Exclusion criteria included pregnancy, breastfeeding, endocrine or chronic diseases (such as diabetes mellitus, cardiovascular disorders, renal disease, and benign or malignant tumors), and the use of hormonal or herbal medications in the past month due to their potential effects on sexual function and androgen levels.
All participants were then asked to complete 2 questionnaires, including a demographic survey and the female sexual function index (FSFI).
Anthropometric measurements -including weight, height, hip circumference (HC), and waist circumference (WC)- were taken by the same trained healthcare professional. Body mass index (BMI) was calculated by dividing weight (kg) by the square of height (m²) to assess obesity. WC was measured at the narrowest point between the lower rib and the iliac crest while standing, and HC was measured at the widest part of the buttocks.
An ovarian volume > 10 ml or containing 12 or more follicles 2-9 mm was distinguished as a positive polycystic ovarian morphology. All required laboratory tests, including testosterone, sex hormone binding globulin (SHBG), were done in the same laboratory (ELISA method).
2.1. Questionnaires
A socio-demographic questionnaire that emphasizes assessing past medical history, menstrual dating and regularity, gynecological history, medications, and family history was completed.
To assess sexual function, all participants were asked to fill out an FSFI questionnaire that included 19 questions to measure women's sexual performance in 6 areas: desire, arousal, lubrication, orgasm, sexual satisfaction, and sexual pain through the Likert scale. The total score was obtained by summing the 6 domain scores. A higher score is associated with a lower degree of sexual dysfunction, and a total score of 23 is the optimal cut score for differentiating women with and without sexual dysfunction. In our study, the FSFI-6 showed high internal consistency with Cronbach’s alpha coefficient of 0.867. The reliability and validity of this questionnaire have been confirmed in Iran (12).
2.2. Sample size
Given that there were no other similar studies in this field, the sample size was determined based on the results of a pilot study (with a sample volume of 60) at a 95% confidence level, using the appropriate formula.
n = ((z1-α/2×S)/d))2 = ((1.96 × 6)/0.5))2
In the above formula, the standard deviation value S from the pilot study and the value Z from the normal distribution table are extracted and replaced, taking into account 95% confidence, and we consider 95% confidence equal to 1.96, and we consider the value d as the accuracy (error) of the estimate.
1-β = 0.90 is power
S = 6 is the standard deviation of sexual function
d = 0.5 is the accuracy of measurement
2.3. Ethical Considerations
This study was approved by the Ethics Committee of Tarbiat Modares University of Medical Sciences, Tehran, Iran (Code: IR.MODARES.REC.1397.211). All procedures were in accordance with the ethical standards of the Regional Research Committee and the Declaration of Helsinki 1964 and its subsequent amendments. Written informed consent and verbal assent were obtained from all participants. In this study, participation was voluntary, confidential, and anonymous, and they had the right to withdraw from the research at any time.
2.4. Statistical Analysis
All data analyses were carried out using Statistical Package for the Social Sciences software (version 25.0) (SPSS, Chicago, IL, USA). Normality was assessed by the Kolmogorov-Smirnov test, and data were presented as Mean + SD for quantitative data, which were compared using Mann-Whitney’s U test. Also, 2 groups were compared in terms of qualitative variables through the Chi-square test, and data were presented as numbers and percentages. P ˂ 0.05 was considered to be statistically significant.
3. Results
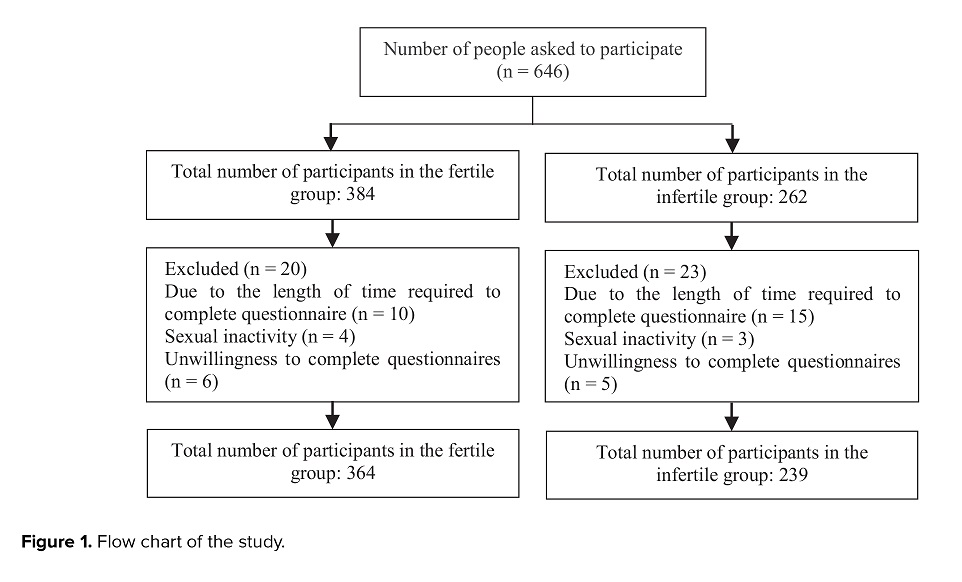
Overall, 25 of the 646 eligible women who were asked to complete the surveys declined to participate in the study due to the length of time required to complete it and the sexual-related content of the questionnaire. A total of 603 women participated in the trial, 18 were excluded due to sexual inactivity (n = 7) and unwillingness to complete questionnaires (n = 11) (Figure 1). The mean age of fertile women was 30.7 5 ± 5.22 yr, and infertile women were 30.76 ± 5.56. Table I shows an overview of some of the main characteristics of the 2 groups. The mean duration of infertility in infertile women was 4.1 ± 3.06 yr, and a significant proportion of infertile women had primary infertility (64.8%). Although no significant difference was observed in the mean level of testosterone between fertile and infertile groups (p = 0.083), SHBG level was significantly different between these groups (p = 0.021).
As can be seen from table II, no significant difference was observed in terms of age (p = 0.904) and BMI (p = 0.908). However, WC and HC were significantly higher in the infertile group (p < 0.001). The 2 groups had significant differences in terms of occupation status and education level, and the level of education in the fertile group was higher than the infertile group (p < 0.001).
Table III provides an evaluation of the 2 groups concerning FSFI. No significant differences were evidenced in terms of the total score (p = 0.391), desire (p = 0.863), arousal (p = 0.405), lubrication (p = 0.583), orgasm (p = 0.901), and satisfaction (p = 0.118) scores. However, pain scores were significantly higher in the fertile women (p < 0.001). The distribution of FSFI domain scores across fertility status categories, including quartiles, is presented in table IV.




4. Discussion
The present study was designed to compare sexual function in fertile and infertile women diagnosed with PCOS according to the Rotterdam criteria. The most interesting finding of this study was that no significant difference was observed between fertile and infertile PCOS women in FSFI characteristics except for pain. The findings of the present study were similar to the results of the study conducted by Oindi et al. (13), who reported that no statistically significant difference was observed in different dimensions of sexual function in fertile and infertile women. Furthermore, another study result showed that both fertile and infertile women had equal incidence of sexual dysfunction, and no significant difference was observed between the 2 groups (14). Also, to investigate the effects of infertility on couples' relationships, some studies have revealed that infertility did not have any significant effect on sexual function and marital relationships. In addition, infertility alone does not increase the risk of sexual dysfunction (15).
Another study found that infertility can affect psychological well-being, marital relationships, sexual relationships, and QoL of couples' lives (16). Furthermore, in a systematic review study, researchers reported a significant reduction in the sexual function of infertile women compared to that of fertile women, with disorders of desire and lubrication being the most common issues among infertile women (17). Also, the researcher argued that although sexual function was significantly different between fertile and infertile women, sexual QoL was the same between these groups (18).
There are various explanations for the inconsistency of the association between infertility and sexual function. For instance, although previous research has shown a significant association between the level of androgens and sexual function (19), in our study, no significant difference was observed between fertile and infertile women in terms of testosterone level. It seems that the results of comparing sexual function between these groups may be affected by this association.
In the present study, SHBG was significantly higher in infertile women, and a recent study reported a significant negative association between sexual desire and SHBG (20). In another study, a similar result was reported, demonstrating that no significant association was observed between serum SHBG levels and female sexual function (21). Different results of the studies mentioned above imply that the relationship between infertility and sexual function is a complex process that might be influenced by multiple factors, including age, economic status, duration of marriage, type of marriage, duration of infertility treatment, and marriage satisfaction (22).
The longer the duration of infertility they face, the more sexual dysfunction they suffer. Moreover, in another study, researchers stated that infertility is one of the most important causes of sexual dysfunction when the duration of infertility exceeds 8 yr (23). In other words, increasing the duration of infertility and unsuccessful treatment reduces the hope of having children and can have adverse effects on sexual function. In our study, the mean duration of infertility in the infertile group was 4.1 ± 3.60, and the effects of infertility on women’s sexual function may be displayed over a longer period. Also, another important factor that can affect sexual function in infertile women is the cause of infertility. Infertile women who have been diagnosed with female infertility, compared to women with unknown causes, are more likely to have sexual dysfunction (24).
Furthermore, older age, self-reported depression, secondary infertility, lower educational level, and higher partner education are further risk factors for female sexual dysfunction in infertile couples.
In our study, the level of education in the fertile group was higher than in the infertile group. Based on the results of some previous studies, it was expected that an increase in education level would be associated with an increase in sexual satisfaction. Also, in the other study, researchers found that the quality of women's sexual life with increasing education levels has shown a statistically significant increase (25). However, the finding that higher levels of education raise women's sexual satisfaction and improve sexual performance has been rejected by some recent studies (26, 27).
Women’s sexual function is related to their mental health status. Depression significantly affects the quality of women's sexual lives (28). The result obtained from a meta-analysis study showed a strong relationship between depression and infertility treatment in infertile women (29). Possible explanations for this association can include experiencing abortion after pregnancy with infertility treatments, the anxiety of high-risk pregnancy, the burden of pregnancy, and the importance of having a child.
Different cultural conditions may explain this inconsistency between the results. Hence, in Eastern societies, fertility and motherhood ability are considered important social and family values, and infertility imposes a psychological burden on individuals (24). What can be deduced from the results of various studies is that although infertility can influence sexual function in various ways, the other manifestations and complications of PCOS and other concurrent factors influence patients' sexual dysfunction.
The results of our study showed that the pain score was significantly higher in the fertile group. Factors that can affect sexual pain in women include younger age, lower BMI, less emotional intimacy with a sexual partner, vaginal infections, especially fungal infections, and severe depression (30).
4.1. Strengths and limitations
In our study, no significant differences were observed between the 2 groups in terms of age and BMI. Still, accurate information on other factors that may affect sexual pain was not available. Consequently, for the best comparison of sexual function between fertile and infertile women with PCOS, evaluation of many factors is required. The main weakness of this study was the paucity of adequate information about women’s mental health status, such as depression, anxiety, the cause and severity of infertility, sexual problems in partners, and the burden of infertility, which could affect their sexual function. Further studies that take these variables into account will need to be undertaken.
5. Conclusion
The present study was designed to evaluate the simultaneous effects of infertility and PCOS on female sexual function. One of the more significant findings to emerge from this study is that infertility is not merely a risk factor for sexual dysfunction without considering other factors. What can be deduced from the results of the present study and several other similar studies in this field is that infertility can affect women’s sexual function. Still, based on the results of other studies discussed in the discussion section, this effect varies depending on various factors that can affect women’s sexual function. Simultaneous review of the results of the present study and other studies conducted in this field shows that, in addition to various individual socio-cultural variables that affect women's sexual function, the effect of factors such as the cause, severity, and duration of infertility, as well as the attitudes of women to their problem, can be different on sexual function. To improve the QoL of infertile women, interventions should be designed and presented by women's health professionals according to the circumstances of each person, while considering these differences.
Data Availability
The data sets used and analyzed for the current study are available upon reasonable request. It will be possible to provide the desired data by contacting the corresponding author.
Author Contributions
Kh. Azarbayjani: Conception and design of the study, literature search, writing the first draft of the manuscript. Sh. Jahanian Sadatmahalleh: Conception and design of the study, literature search, statistical analysis, writing the first draft of the manuscript. N. Mirzaei: Literature search, statistical analysis, writing the first draft of the manuscript. N. Jahangiri: Literature search, writing the first draft of the manuscript. M. Nasiri: Statistical analysis, wrote the first draft of the manuscript. M. Yarjanli: Conception and design of the study, literature search ,data collection. M. Zeinaloo: Data collection, literature search. Sh. Jahanian Sadatmahalleh, Kh. Azarbayjani and M. Yarjanli contributed to the conception and design of the study; Kh. Azarbayjani, N. Mirzaei, N. Jahangiri, M. Yarjanli, M. Zeinaloo: and Sh. Jahanian Sadatmahalleh did the literature search; M. Nasiri, N. Mirzaei, and Sh. Jahanian Sadatmahalleh: Performed the statistical analysis; Kh. Azarbayjani, N. Mirzaei, Sh. Jahanian Sadatmahalleh, N. Jahangiri, and M. Nasiri wrote the first draft of the manuscript. All authors contributed to the manuscript revision, and read and approved the submitted version.
Acknowledgments
This study was carried out with the collaboration of the participants and was not financially supported. Artificial intelligence was not used in the present study.
Conflict of Interest
The authors declare that there is no conflict of interest.
Polycystic ovarian syndrome (PCOS) is a complex endocrine disorder that affects approximately 9.2% of women of reproductive age globally (1). Ovulatory dysfunction and hyperandrogenism, which includes hirsutism, acne, obesity, and polycystic ovarian morphology, are characteristic of this condition (2).
Furthermore, infertility is defined as the inability to conceive after 1 yr of regular intercourse without contraception, which affects 70-80% of women with PCOS (3). Infertility is a risk factor for sexual dysfunction, as 5-55% of infertile women experience it (4). Infertility not only has a devastating effect on patients' self-esteem but also imposes a lot of financial and psychological burdens on them, consequently, infertility may affect couples' relationships and their satisfaction with sexual intercourse (5). It seems that PCOS is associated with an increased risk of sexual dysfunction as follows: aesthetic factors such as hirsutism, acne, and obesity change the women’s attitude toward their bodies, leading to diminished feminine identity. Imbalance in hormonal profile, hyperandrogenism, and hyperinsulinemia can lead to depression and anxiety that have manifold effects on quality of life (QoL), mental health, and consequently change women’s sexual function (6).
Although in many studies, it is proven that infertility is strongly related to impaired sexual dysfunction, data on the association between sexual function and PCOS are limited and often contradicting (7-10). Thus, in light of previous studies on the detrimental effects of infertility and PCOS on sexual function and the synergistic effects that infertility and PCOS have on each other, infertile PCOS patients might suffer from sexual dysfunction markedly as a comorbidity.
Given the higher prevalence of infertility in women with PCOS, the present study aimed to investigate and compare sexual function as one of the important aspects of women’s lives. The results of the present study, by examining the effects of infertility on women's sexual function, can be used as part of counseling and treatment measures for these patients to reduce the complications of the disease in women with PCOS.
A previous version of this manuscript was presented as a preprint on ResearchSquare prior to peer review. The current version has been revised based on feedback from the peer-review process.
2. Materials and Methods
In this cross-sectional study, 603 women with PCOS who were referred to the Arash hospital gynecological clinics affiliated with Tehran University of Medical Sciences, Tehran, Iran between April 2019 and February 2020 were enrolled through a convenience sampling method. They were categorized into 2 groups: fertile (n = 364) and infertile (n = 239).
Inclusion criteria: married women diagnosed with PCOS based on the Rotterdam criteria (11), aged 18-45 yr, and sexually active in the past 4 wk. Infertility was defined as the inability to conceive after 12 months or more of regular unprotected intercourse, including both primary and secondary infertility.
Exclusion criteria included pregnancy, breastfeeding, endocrine or chronic diseases (such as diabetes mellitus, cardiovascular disorders, renal disease, and benign or malignant tumors), and the use of hormonal or herbal medications in the past month due to their potential effects on sexual function and androgen levels.
All participants were then asked to complete 2 questionnaires, including a demographic survey and the female sexual function index (FSFI).
Anthropometric measurements -including weight, height, hip circumference (HC), and waist circumference (WC)- were taken by the same trained healthcare professional. Body mass index (BMI) was calculated by dividing weight (kg) by the square of height (m²) to assess obesity. WC was measured at the narrowest point between the lower rib and the iliac crest while standing, and HC was measured at the widest part of the buttocks.
An ovarian volume > 10 ml or containing 12 or more follicles 2-9 mm was distinguished as a positive polycystic ovarian morphology. All required laboratory tests, including testosterone, sex hormone binding globulin (SHBG), were done in the same laboratory (ELISA method).
2.1. Questionnaires
A socio-demographic questionnaire that emphasizes assessing past medical history, menstrual dating and regularity, gynecological history, medications, and family history was completed.
To assess sexual function, all participants were asked to fill out an FSFI questionnaire that included 19 questions to measure women's sexual performance in 6 areas: desire, arousal, lubrication, orgasm, sexual satisfaction, and sexual pain through the Likert scale. The total score was obtained by summing the 6 domain scores. A higher score is associated with a lower degree of sexual dysfunction, and a total score of 23 is the optimal cut score for differentiating women with and without sexual dysfunction. In our study, the FSFI-6 showed high internal consistency with Cronbach’s alpha coefficient of 0.867. The reliability and validity of this questionnaire have been confirmed in Iran (12).
2.2. Sample size
Given that there were no other similar studies in this field, the sample size was determined based on the results of a pilot study (with a sample volume of 60) at a 95% confidence level, using the appropriate formula.
n = ((z1-α/2×S)/d))2 = ((1.96 × 6)/0.5))2
In the above formula, the standard deviation value S from the pilot study and the value Z from the normal distribution table are extracted and replaced, taking into account 95% confidence, and we consider 95% confidence equal to 1.96, and we consider the value d as the accuracy (error) of the estimate.
1-β = 0.90 is power
S = 6 is the standard deviation of sexual function
d = 0.5 is the accuracy of measurement
2.3. Ethical Considerations
This study was approved by the Ethics Committee of Tarbiat Modares University of Medical Sciences, Tehran, Iran (Code: IR.MODARES.REC.1397.211). All procedures were in accordance with the ethical standards of the Regional Research Committee and the Declaration of Helsinki 1964 and its subsequent amendments. Written informed consent and verbal assent were obtained from all participants. In this study, participation was voluntary, confidential, and anonymous, and they had the right to withdraw from the research at any time.
2.4. Statistical Analysis
All data analyses were carried out using Statistical Package for the Social Sciences software (version 25.0) (SPSS, Chicago, IL, USA). Normality was assessed by the Kolmogorov-Smirnov test, and data were presented as Mean + SD for quantitative data, which were compared using Mann-Whitney’s U test. Also, 2 groups were compared in terms of qualitative variables through the Chi-square test, and data were presented as numbers and percentages. P ˂ 0.05 was considered to be statistically significant.
3. Results
Overall, 25 of the 646 eligible women who were asked to complete the surveys declined to participate in the study due to the length of time required to complete it and the sexual-related content of the questionnaire. A total of 603 women participated in the trial, 18 were excluded due to sexual inactivity (n = 7) and unwillingness to complete questionnaires (n = 11) (Figure 1). The mean age of fertile women was 30.7 5 ± 5.22 yr, and infertile women were 30.76 ± 5.56. Table I shows an overview of some of the main characteristics of the 2 groups. The mean duration of infertility in infertile women was 4.1 ± 3.06 yr, and a significant proportion of infertile women had primary infertility (64.8%). Although no significant difference was observed in the mean level of testosterone between fertile and infertile groups (p = 0.083), SHBG level was significantly different between these groups (p = 0.021).
As can be seen from table II, no significant difference was observed in terms of age (p = 0.904) and BMI (p = 0.908). However, WC and HC were significantly higher in the infertile group (p < 0.001). The 2 groups had significant differences in terms of occupation status and education level, and the level of education in the fertile group was higher than the infertile group (p < 0.001).
Table III provides an evaluation of the 2 groups concerning FSFI. No significant differences were evidenced in terms of the total score (p = 0.391), desire (p = 0.863), arousal (p = 0.405), lubrication (p = 0.583), orgasm (p = 0.901), and satisfaction (p = 0.118) scores. However, pain scores were significantly higher in the fertile women (p < 0.001). The distribution of FSFI domain scores across fertility status categories, including quartiles, is presented in table IV.





4. Discussion
The present study was designed to compare sexual function in fertile and infertile women diagnosed with PCOS according to the Rotterdam criteria. The most interesting finding of this study was that no significant difference was observed between fertile and infertile PCOS women in FSFI characteristics except for pain. The findings of the present study were similar to the results of the study conducted by Oindi et al. (13), who reported that no statistically significant difference was observed in different dimensions of sexual function in fertile and infertile women. Furthermore, another study result showed that both fertile and infertile women had equal incidence of sexual dysfunction, and no significant difference was observed between the 2 groups (14). Also, to investigate the effects of infertility on couples' relationships, some studies have revealed that infertility did not have any significant effect on sexual function and marital relationships. In addition, infertility alone does not increase the risk of sexual dysfunction (15).
Another study found that infertility can affect psychological well-being, marital relationships, sexual relationships, and QoL of couples' lives (16). Furthermore, in a systematic review study, researchers reported a significant reduction in the sexual function of infertile women compared to that of fertile women, with disorders of desire and lubrication being the most common issues among infertile women (17). Also, the researcher argued that although sexual function was significantly different between fertile and infertile women, sexual QoL was the same between these groups (18).
There are various explanations for the inconsistency of the association between infertility and sexual function. For instance, although previous research has shown a significant association between the level of androgens and sexual function (19), in our study, no significant difference was observed between fertile and infertile women in terms of testosterone level. It seems that the results of comparing sexual function between these groups may be affected by this association.
In the present study, SHBG was significantly higher in infertile women, and a recent study reported a significant negative association between sexual desire and SHBG (20). In another study, a similar result was reported, demonstrating that no significant association was observed between serum SHBG levels and female sexual function (21). Different results of the studies mentioned above imply that the relationship between infertility and sexual function is a complex process that might be influenced by multiple factors, including age, economic status, duration of marriage, type of marriage, duration of infertility treatment, and marriage satisfaction (22).
The longer the duration of infertility they face, the more sexual dysfunction they suffer. Moreover, in another study, researchers stated that infertility is one of the most important causes of sexual dysfunction when the duration of infertility exceeds 8 yr (23). In other words, increasing the duration of infertility and unsuccessful treatment reduces the hope of having children and can have adverse effects on sexual function. In our study, the mean duration of infertility in the infertile group was 4.1 ± 3.60, and the effects of infertility on women’s sexual function may be displayed over a longer period. Also, another important factor that can affect sexual function in infertile women is the cause of infertility. Infertile women who have been diagnosed with female infertility, compared to women with unknown causes, are more likely to have sexual dysfunction (24).
Furthermore, older age, self-reported depression, secondary infertility, lower educational level, and higher partner education are further risk factors for female sexual dysfunction in infertile couples.
In our study, the level of education in the fertile group was higher than in the infertile group. Based on the results of some previous studies, it was expected that an increase in education level would be associated with an increase in sexual satisfaction. Also, in the other study, researchers found that the quality of women's sexual life with increasing education levels has shown a statistically significant increase (25). However, the finding that higher levels of education raise women's sexual satisfaction and improve sexual performance has been rejected by some recent studies (26, 27).
Women’s sexual function is related to their mental health status. Depression significantly affects the quality of women's sexual lives (28). The result obtained from a meta-analysis study showed a strong relationship between depression and infertility treatment in infertile women (29). Possible explanations for this association can include experiencing abortion after pregnancy with infertility treatments, the anxiety of high-risk pregnancy, the burden of pregnancy, and the importance of having a child.
Different cultural conditions may explain this inconsistency between the results. Hence, in Eastern societies, fertility and motherhood ability are considered important social and family values, and infertility imposes a psychological burden on individuals (24). What can be deduced from the results of various studies is that although infertility can influence sexual function in various ways, the other manifestations and complications of PCOS and other concurrent factors influence patients' sexual dysfunction.
The results of our study showed that the pain score was significantly higher in the fertile group. Factors that can affect sexual pain in women include younger age, lower BMI, less emotional intimacy with a sexual partner, vaginal infections, especially fungal infections, and severe depression (30).
4.1. Strengths and limitations
In our study, no significant differences were observed between the 2 groups in terms of age and BMI. Still, accurate information on other factors that may affect sexual pain was not available. Consequently, for the best comparison of sexual function between fertile and infertile women with PCOS, evaluation of many factors is required. The main weakness of this study was the paucity of adequate information about women’s mental health status, such as depression, anxiety, the cause and severity of infertility, sexual problems in partners, and the burden of infertility, which could affect their sexual function. Further studies that take these variables into account will need to be undertaken.
5. Conclusion
The present study was designed to evaluate the simultaneous effects of infertility and PCOS on female sexual function. One of the more significant findings to emerge from this study is that infertility is not merely a risk factor for sexual dysfunction without considering other factors. What can be deduced from the results of the present study and several other similar studies in this field is that infertility can affect women’s sexual function. Still, based on the results of other studies discussed in the discussion section, this effect varies depending on various factors that can affect women’s sexual function. Simultaneous review of the results of the present study and other studies conducted in this field shows that, in addition to various individual socio-cultural variables that affect women's sexual function, the effect of factors such as the cause, severity, and duration of infertility, as well as the attitudes of women to their problem, can be different on sexual function. To improve the QoL of infertile women, interventions should be designed and presented by women's health professionals according to the circumstances of each person, while considering these differences.
Data Availability
The data sets used and analyzed for the current study are available upon reasonable request. It will be possible to provide the desired data by contacting the corresponding author.
Author Contributions
Kh. Azarbayjani: Conception and design of the study, literature search, writing the first draft of the manuscript. Sh. Jahanian Sadatmahalleh: Conception and design of the study, literature search, statistical analysis, writing the first draft of the manuscript. N. Mirzaei: Literature search, statistical analysis, writing the first draft of the manuscript. N. Jahangiri: Literature search, writing the first draft of the manuscript. M. Nasiri: Statistical analysis, wrote the first draft of the manuscript. M. Yarjanli: Conception and design of the study, literature search ,data collection. M. Zeinaloo: Data collection, literature search. Sh. Jahanian Sadatmahalleh, Kh. Azarbayjani and M. Yarjanli contributed to the conception and design of the study; Kh. Azarbayjani, N. Mirzaei, N. Jahangiri, M. Yarjanli, M. Zeinaloo: and Sh. Jahanian Sadatmahalleh did the literature search; M. Nasiri, N. Mirzaei, and Sh. Jahanian Sadatmahalleh: Performed the statistical analysis; Kh. Azarbayjani, N. Mirzaei, Sh. Jahanian Sadatmahalleh, N. Jahangiri, and M. Nasiri wrote the first draft of the manuscript. All authors contributed to the manuscript revision, and read and approved the submitted version.
Acknowledgments
This study was carried out with the collaboration of the participants and was not financially supported. Artificial intelligence was not used in the present study.
Conflict of Interest
The authors declare that there is no conflict of interest.
Type of Study: Original Article |
Subject:
Fertility & Infertility
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |




