Fri, May 8, 2026
[Archive]
Volume 20, Issue 1 (January 2022)
IJRM 2022, 20(1): 13-20 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Azin F, Khazali H. Phytotherapy of polycystic ovary syndrome: A review. IJRM 2022; 20 (1) :13-20
URL: http://ijrm.ir/article-1-1878-en.html
URL: http://ijrm.ir/article-1-1878-en.html
1- Department of Animal Science and Biotechnology, Faculty of Life Sciences and Biotechnology, Shahid Beheshti University, Tehran, Iran. , f_azin@yahoo.com
2- Department of Animal Science and Biotechnology, Faculty of Life Sciences and Biotechnology, Shahid Beheshti University, Tehran, Iran.
2- Department of Animal Science and Biotechnology, Faculty of Life Sciences and Biotechnology, Shahid Beheshti University, Tehran, Iran.
Full-Text [PDF 281 kb]
(2481 Downloads)
| Abstract (HTML) (3818 Views)
1. Introduction
Polycystic ovary syndrome (PCOS) is a heterogeneous endocrine disease with various symptoms, which affects 5-10% of females of reproductive age (1, 2). The main clinical features of PCOS are being over-weight, hyperandrogenaemia, polycystic ovarian morphology and hyperinsulinemia (3). Although the etiology of PCOS is not completely understood yet, scientific studies suggest that uncontrolled steroidogenesis may be the primary feature in this syndrome (4). PCOS, as a complex heterogeneous disease, can be associated with various genetic, metabolic, endocrine and environmental abnormalities such as over-weight and obesity, type 2 diabetes, impaired glucose tolerance, insulin resistance, hyperandrogenism and increased luteinizing hormone (LH) (5, 6).
Increases in oxidative stress levels and inflammatory markers, LH and androgens, and a significant reduction in follicle stimulating hormone (FSH) and estrogen have been reported in patients with PCOS and also in animal models of PCOS (7, 8). It has been shown that non-chemical and herbal ingredients can have considerable effects on recovery and improvement of some abnormalities and disorders in PCOS patients, and many studies have been conducted on their effects on the hormonal and metabolic factors and hypothalamic-pituitary-ovarian axis in PCOS (9-42).
This review summarizes the studies conducted over a given period that show the efficacy of these non-chemical and herbal substances in treating PCOS.
2. Materials and Methods
This review was carried out using relevant keywords in the electronic databases PubMed/MEDLINE, Web of Science, Scopus and Reaxys. Articles were limited to those published from January 2009 to December 2019 and we used the keywords “non-chemical treatment”, “herbal treatment”, “phytotherapy”, “polycystic ovary syndrome” and “PCOS”. We conducted searches to capture all animal studies and pre-clinical and clinical studies explaining the effects of herbal extracts on PCOS. In addition, we manually searched bibliographies of review articles. A total of 230 studies were found to be about the effects of herbal compositions on the treatment of PCOS. We excluded clinical and animal studies investigating herbal medicines with unrelated outcomes and finally 34 studies were selected.
3. Results
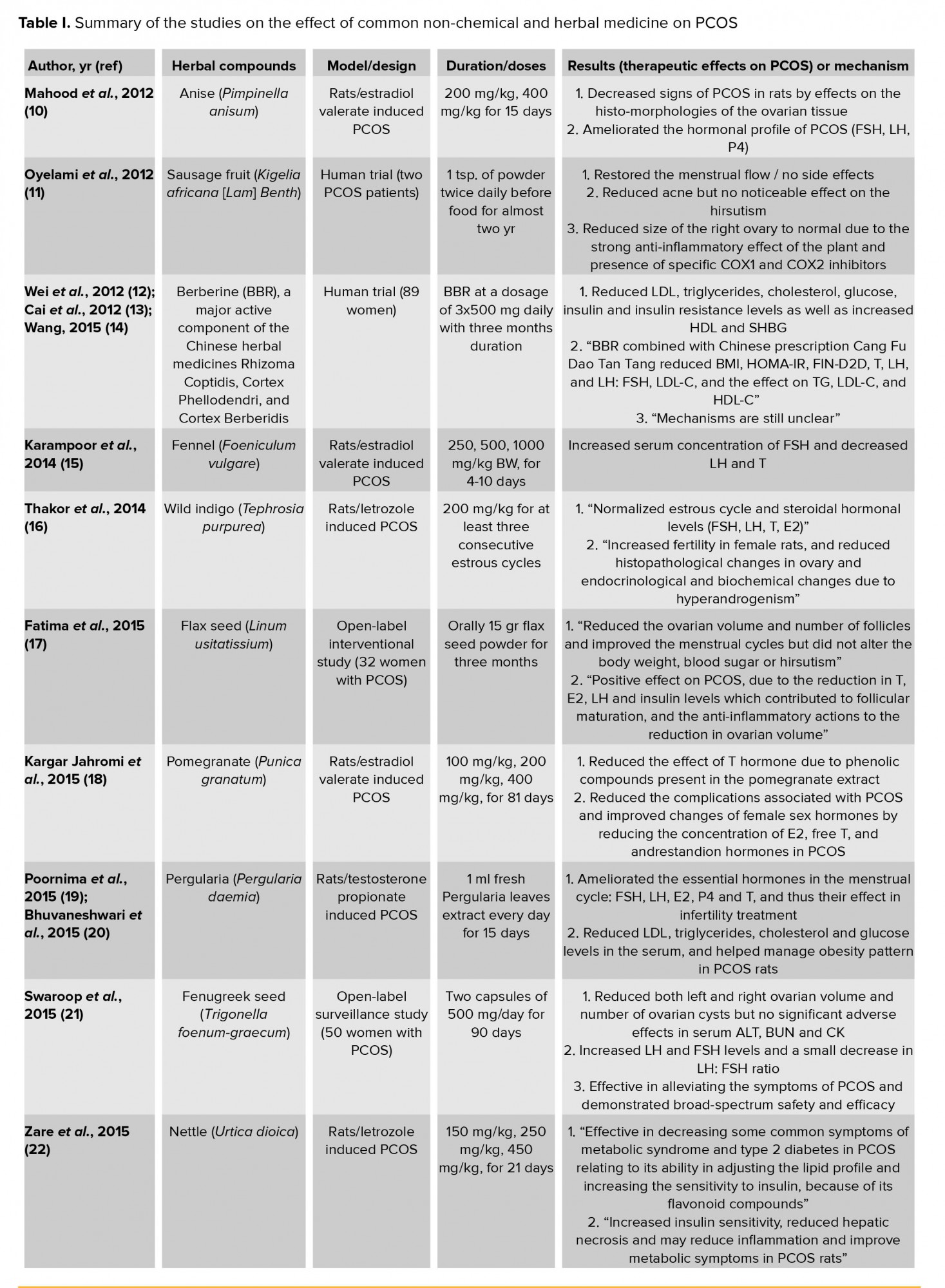
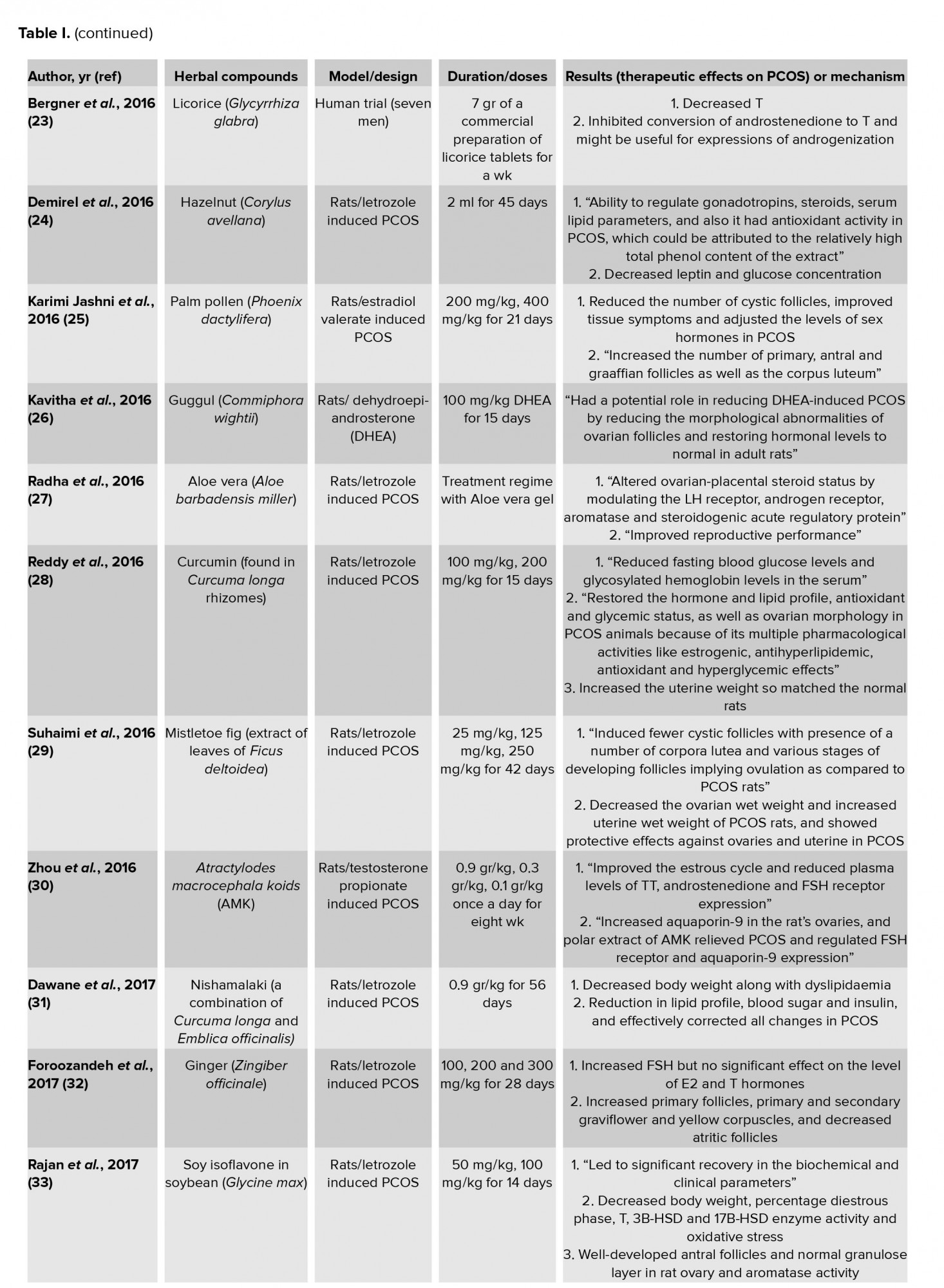
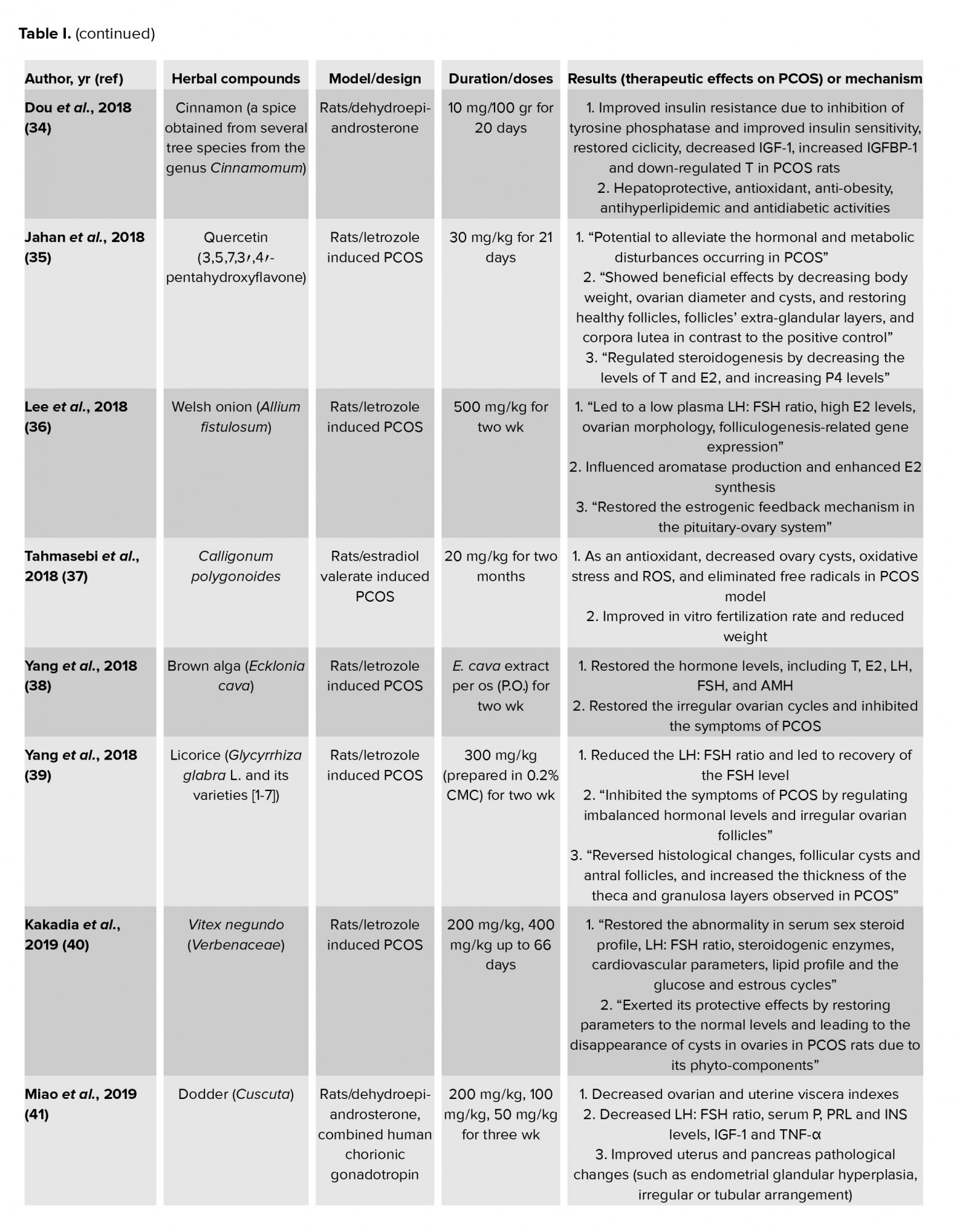
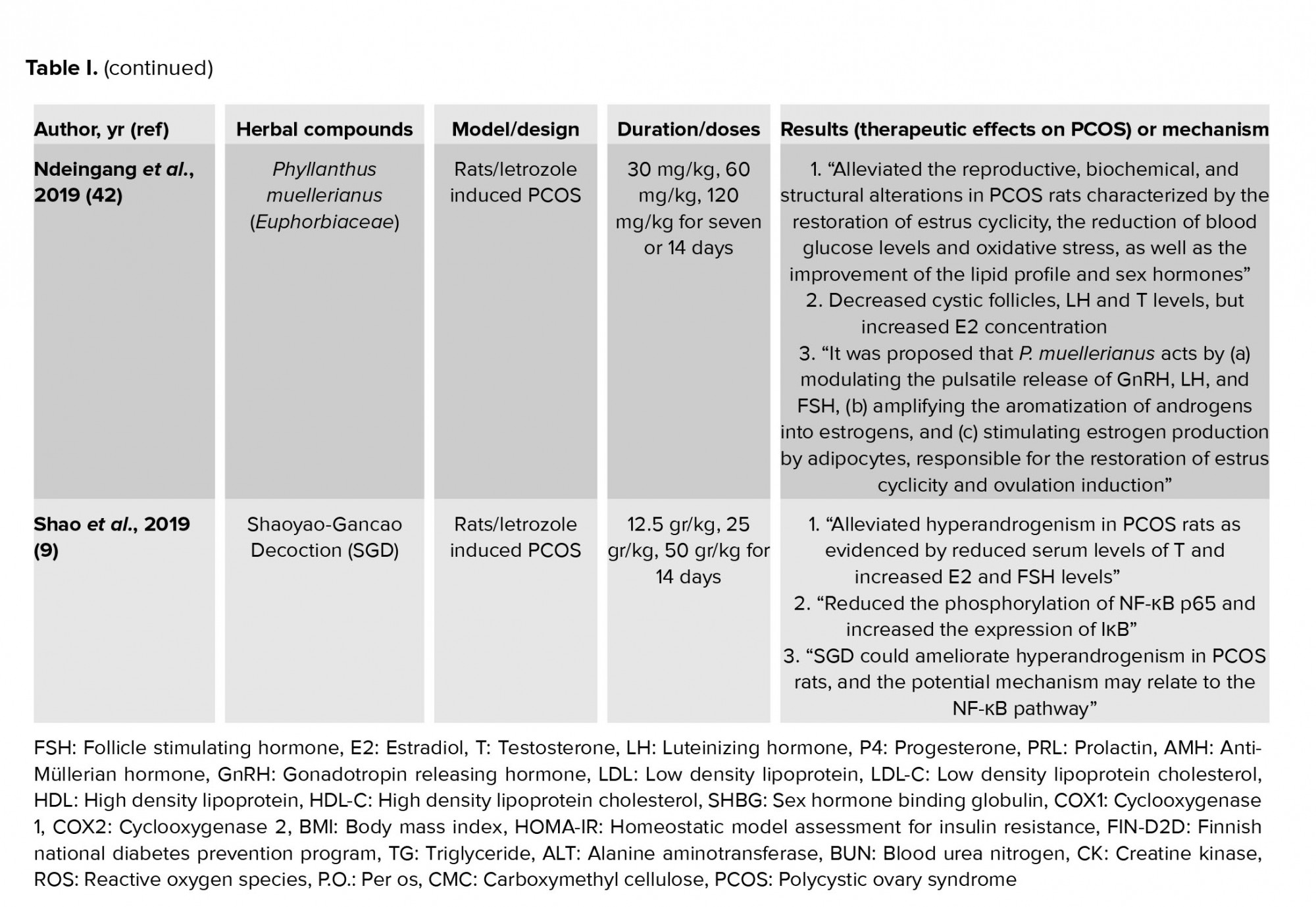
There have been numerous studies on the etiology of PCOS and its common and traditional herbal and non-chemical treatments (1-47). Each of these treatments has different effects. Most of them can partially improve metabolic and hormonal abnormalities. This can be an effective way for preventing and treating PCOS by affecting the factors involved in the disease. Some important experimental studies with significant results and human and clinical trials are described in table I. In most of these studies, the regulation and balance of the steroidogenic enzymes, sex steroid profile, LH: FSH ratio, lipid profile, glucose or insulin levels were reported, which aimed to improve and treat PCOS disease.
4. Discussion
This review lists laboratory, clinical, and animal studies which used phytotherapy to treat PCOS disease (9-42). The results demonstrated the importance and potential of herbal and non-chemical therapies to improve the hormonal status such as FSH, LH, their ratios and significant recovery in the biochemical and clinical parameters of PCOS. For example, in one study this was done through restoring the estrus cyclicity, decreasing cystic follicles, LH and testosterone levels, and increasing estradiol and FSH concentrations in PCOS rats treated with Phyllanthus muellerianus (Euphorbiaceae) (42). Another example was Berberine, which in human trials, combined with Chinese herbs, showed positive effects on alleviating insulin resistance, and improving glycolipid metabolism and reproductive endocrine conditions (43).
Since there are different results from different herbal compounds in these studies, it is necessary to classify herbal compounds according to the hormonal and neurological factors and changes in gene expression level. A number of herbal compounds and substances can be given more attention as they control and influence hormones at the level of the central nervous system and its major axes in the reproductive system, including testosterone, estrogen, LH and FSH (9, 32, 38, 39, 41, 42). In some studies, the effect of neuropeptides such as from the galanin family have been evaluated in the treatment of PCOS disease (44, 45). PCOS patients have been shown to have significantly lower levels of nesfatin-1 (45) and also one study showed a small increase in galanin, but this was not significant compared to the control group (46). Recently, we demonstrated that galanin as a neuropeptide could ameliorate the metabolic and reproductive disturbances in a rat model of PCOS (47).
Determining the exact causes of the disease and its molecular basis can certainly play a key role in the treatment of PCOS using non-chemical & herbal ingredients and neuropeptides. Further pre-clinical, clinical and experimental studies are needed to show the effects of these non-chemical components for the management of PCOS.
5. Conclusion
This review demonstrated the variability and effects of phytotherapy and non-chemical treatments associated with PCOS disease. These findings may help future studies on the etiology and treatment of this syndrome, which is the most common cause of female infertility.
Acknowledgments
The authors acknowledge the central library of Shahid Beheshti University, Tehran, Iran for helping to access the data and original scientific articles.
Conflict of Interest
The authors declare that there is no conflict of interest.
Full-Text: (844 Views)
1. Introduction
Polycystic ovary syndrome (PCOS) is a heterogeneous endocrine disease with various symptoms, which affects 5-10% of females of reproductive age (1, 2). The main clinical features of PCOS are being over-weight, hyperandrogenaemia, polycystic ovarian morphology and hyperinsulinemia (3). Although the etiology of PCOS is not completely understood yet, scientific studies suggest that uncontrolled steroidogenesis may be the primary feature in this syndrome (4). PCOS, as a complex heterogeneous disease, can be associated with various genetic, metabolic, endocrine and environmental abnormalities such as over-weight and obesity, type 2 diabetes, impaired glucose tolerance, insulin resistance, hyperandrogenism and increased luteinizing hormone (LH) (5, 6).
Increases in oxidative stress levels and inflammatory markers, LH and androgens, and a significant reduction in follicle stimulating hormone (FSH) and estrogen have been reported in patients with PCOS and also in animal models of PCOS (7, 8). It has been shown that non-chemical and herbal ingredients can have considerable effects on recovery and improvement of some abnormalities and disorders in PCOS patients, and many studies have been conducted on their effects on the hormonal and metabolic factors and hypothalamic-pituitary-ovarian axis in PCOS (9-42).
This review summarizes the studies conducted over a given period that show the efficacy of these non-chemical and herbal substances in treating PCOS.
2. Materials and Methods
This review was carried out using relevant keywords in the electronic databases PubMed/MEDLINE, Web of Science, Scopus and Reaxys. Articles were limited to those published from January 2009 to December 2019 and we used the keywords “non-chemical treatment”, “herbal treatment”, “phytotherapy”, “polycystic ovary syndrome” and “PCOS”. We conducted searches to capture all animal studies and pre-clinical and clinical studies explaining the effects of herbal extracts on PCOS. In addition, we manually searched bibliographies of review articles. A total of 230 studies were found to be about the effects of herbal compositions on the treatment of PCOS. We excluded clinical and animal studies investigating herbal medicines with unrelated outcomes and finally 34 studies were selected.
3. Results
There have been numerous studies on the etiology of PCOS and its common and traditional herbal and non-chemical treatments (1-47). Each of these treatments has different effects. Most of them can partially improve metabolic and hormonal abnormalities. This can be an effective way for preventing and treating PCOS by affecting the factors involved in the disease. Some important experimental studies with significant results and human and clinical trials are described in table I. In most of these studies, the regulation and balance of the steroidogenic enzymes, sex steroid profile, LH: FSH ratio, lipid profile, glucose or insulin levels were reported, which aimed to improve and treat PCOS disease.




4. Discussion
This review lists laboratory, clinical, and animal studies which used phytotherapy to treat PCOS disease (9-42). The results demonstrated the importance and potential of herbal and non-chemical therapies to improve the hormonal status such as FSH, LH, their ratios and significant recovery in the biochemical and clinical parameters of PCOS. For example, in one study this was done through restoring the estrus cyclicity, decreasing cystic follicles, LH and testosterone levels, and increasing estradiol and FSH concentrations in PCOS rats treated with Phyllanthus muellerianus (Euphorbiaceae) (42). Another example was Berberine, which in human trials, combined with Chinese herbs, showed positive effects on alleviating insulin resistance, and improving glycolipid metabolism and reproductive endocrine conditions (43).
Since there are different results from different herbal compounds in these studies, it is necessary to classify herbal compounds according to the hormonal and neurological factors and changes in gene expression level. A number of herbal compounds and substances can be given more attention as they control and influence hormones at the level of the central nervous system and its major axes in the reproductive system, including testosterone, estrogen, LH and FSH (9, 32, 38, 39, 41, 42). In some studies, the effect of neuropeptides such as from the galanin family have been evaluated in the treatment of PCOS disease (44, 45). PCOS patients have been shown to have significantly lower levels of nesfatin-1 (45) and also one study showed a small increase in galanin, but this was not significant compared to the control group (46). Recently, we demonstrated that galanin as a neuropeptide could ameliorate the metabolic and reproductive disturbances in a rat model of PCOS (47).
Determining the exact causes of the disease and its molecular basis can certainly play a key role in the treatment of PCOS using non-chemical & herbal ingredients and neuropeptides. Further pre-clinical, clinical and experimental studies are needed to show the effects of these non-chemical components for the management of PCOS.
5. Conclusion
This review demonstrated the variability and effects of phytotherapy and non-chemical treatments associated with PCOS disease. These findings may help future studies on the etiology and treatment of this syndrome, which is the most common cause of female infertility.
Acknowledgments
The authors acknowledge the central library of Shahid Beheshti University, Tehran, Iran for helping to access the data and original scientific articles.
Conflict of Interest
The authors declare that there is no conflict of interest.
Type of Study: Review Article |
Subject:
Reproductive Endocrinology
References
1. Franks S. Polycystic ovary syndrome. N Engl J Med 1995; 333: 853-861. [DOI:10.1056/NEJM199509283331307] [PMID]
2. Ihsan I, Tehreem A, Rasool S. Significance of TNF-alpha and insulin resistance in women with polycystic ovarian syndrome. Pakistan J Med Health Sci 2018; 12: 459-463.
3. Rotterdam ESHRE/ASRM-sponsored PCOS consensus workshop group. Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome. Fertil Steril 2004; 81: 19-25. [DOI:10.1016/j.fertnstert.2003.10.004]
4. Walters KA, Rodriguez Paris V, Aflatounian A, Handelsman DJ. Androgens and ovarian function: Translation from basic diversity research to clinical impact. J Endocrinol 2019; 242: 23-50. [DOI:10.1530/JOE-19-0096] [PMID]
5. Norman RJ, Dewailly D, Legro RS, Hickey TE. Polycystic ovary syndrome. Lancet 2007; 370: 685-697. [DOI:10.1016/S0140-6736(07)61345-2]
6. Szczuko M, Zapalowska-Chwyc M, Drozd A, Maciejewska D, Starczewski A, Stachowska E. Effect of IGF-I and TNF-α on intensification of steroid pathways in women with PCOS phenotypes are not identical: Enhancement of progesterone pathway in women with PCOS increases the concentration of TNF-α. Gynecol Endocrinol 2016; 32: 714-717. [DOI:10.3109/09513590.2016.1159672] [PMID]
7. Sabuncu T, Vural H, Harma M, Harma M. Oxidative stress in polycystic ovary syndrome and its contribution to the risk of cardiovascular disease. Clin Biochem 2001; 34: 407-413. [DOI:10.1016/S0009-9120(01)00245-4]
8. De Leo V, Musacchio MC, Cappelli V, Massaro MG, Morgante G, Petraglia F. Genetic, hormonal and metabolic aspects of PCOS: An update. Reprod Biol Endocrinol 2016; 14: 38-54. [DOI:10.1186/s12958-016-0173-x] [PMID] [PMCID]
9. Shao YY, Chang ZhP, Cheng Y, Wang XCh, Zhang JP, Feng XJ, et al. Shaoyao-gancao decoction alleviated hyperandrogenism in a letrozole-induced rat model of polycystic ovary syndrome by inhibition of NF-κB activation. Biosci Rep 2019; 39: BSR20181877. [DOI:10.1042/BSR20181877] [PMID] [PMCID]
10. Mahood RAH. Effects of Pimpinella anisum oil extract on some biochemical parameters in mice experimentally induced for human polycystic ovary syndrome. J Biotech Res Centre 2012; 6: 67-73. [DOI:10.24126/jobrc.2012.6.2.228]
11. Oyelami OA, Yusuf KO, Oyelami AO. The use of kigelia africana in the management of polycystic ovary syndrome (PCOS). Chinese Med 2012; 3: 1-3. [DOI:10.4236/cm.2012.31001]
12. Wei W, Zhao H, Wang A, Sui M, Liang K, Deng H, et al. A clinical study on the short-term effect of berberine in comparison to metformin on the metabolic characteristics of women with polycystic ovary syndrome. Eur J Endocrinol 2012; 166: 99-105. [DOI:10.1530/EJE-11-0616] [PMID]
13. Cai L. Clinical treatment of polycystic ovary syndrome of combination use of Gui Zhi Fu Ling Wan and berberine. Henan J Surg 2012; 18: 60-62.
14. Wang Y. The clinical study on the effect of Berberine combined with Cang-Fu-Dao-Tan decoction treating obese women with polycystic ovary syndrome. Guangzhuo Univ Chinese Med 2015.
15. Karampoor P, Azarnia M, Mirabolghasemi Gh, Alizadeh F. [The effect of hydroalcoholic extract of fennel (Foeniculum vulgare) seed on serum levels of sexual hormones in female Wistar rats with polycystic ovarian syndrome (PCOS)]. J Arak Univ Med Sci 2014; 17: 70-78. (in Persian)
16. Thakor AP, Patel AJ. Normalizing of the oestrous cycle in polycystic ovary syndrome (PCOS) induced rats with Tephrosia purpurea (Linn.) pers. J Appl Nat Sci 2014; 6: 197-201. [DOI:10.31018/jans.v6i1.400]
17. Fatima Farzana K, Abubacker Sulaiman F, Ruckmani A, Vijayalakshmi K, Karunya Lakshmi G, Shri Ranjini S, et al. Effects of flax seeds supplementation in polycystic ovarian syndrome. Int J Pharm Sci Rev Res 2015; 31: 113-119.
18. Kargar Jahromi H, Kargar L, Tavakol koukhdan E, Shfiei Jahromi N, Poorgholami F, Rahmanian E, et al. The effect of pomegranate juice extract on hormonal changes of female Wistar rats caused by polycystic. Biomed Pharmacol J 2015; 8: 971-977. [DOI:10.13005/bpj/849]
19. Poornima R, Saranya M, Bhuvaneshwari S, Averal HI. Evaluation of pregularia daemia and metformin in the treatment of PCOS in testosterone propionate induced albino wistar rats (Rattus norvegicus). Int J Pharma Sci Res 2015; 6: 1250-1256.
20. Bhuvaneshwari S, Poornima R, Averal HI. Comparitive study of pergularia daemia and citrullus colocynthis in polycystic ovarian syndrome induced albino Wistar rats. Int J Multidisc Res Dev 2015; 2: 207-212.
21. Swaroop A, Jaipuriar AS, Gupta SK, Bagchi M, Kumar P, Preuss HG, et al. Efficacy of a novel fenugreek seed extract (trigonella foenum-graecum, furocyst TM) in polycystic ovary syndrome (PCOS). Int J Med Sci 2015; 12: 825-831. [DOI:10.7150/ijms.13024] [PMID] [PMCID]
22. Zare S, Nabiuni M, Tayanloo A, Hoseini S, Karimzadeh-Bardei L. The effects of urtica dioica extract on lipid profile, insulin resistance index and liver histology in polycystic ovary syndrome-induced Wistar rats. Adv Herb Med 2015; 1: 23-33.
23. Bergner P. Glycyrrhiza: Licorice root and testosterone. Med Herb 2016; 11: 11-12.
24. Demirel MA, Ilhan M, Suntar I, Keles H, Akkol EK. Activity of Corylus avellana seed oil in letrozole-induced polycystic ovary syndrome model in rats. Revista Brasileira de Farmacognosia 2016; 26: 83-88. [DOI:10.1016/j.bjp.2015.09.009]
25. Karimi Jashni H, Karegar Jahromi H, Bagheri Z. The effect of palm pollen extracts on polycystic ovary syndrome (POS) in rats. Int J Med Res Health Sci 2016; 5: 317-321.
26. Kavitha A, Babu AN, Kumar MS, Kiran SV. Evaluation of effect of commiphora wightii in dehydroepiandrosterone (DHEA) induced polycystic ovary syndrome (PCOS) in rats. Pharm Tutor 2016; 4: 47-55.
27. Radha MH, Laxmipriya NP. The role of aloe barbadensis mill as a possible pre-conceptive herb for the management of polycystic ovarian syndrome : A rodent model study. Austin J Reprod Med Infertil 2016; 3: 1040-1048.
28. Reddy PS, Begum N, Mutha S, Bakshi V. Beneficial effect of curcumin in letrozole induced polycystic ovary syndrome. Asian Pac J Reprod 2016; 5: 116-122. [DOI:10.1016/j.apjr.2016.01.006]
29. Suhaimi NA, Nooraain H, Nurdiana S. Effects of ficus deltoidea ethanolic leaves extract on female reproductive organs among letrozole‐induced polycystic ovarian syndrome rats. J Sci Res Dev 2016; 3: 8-14.
30. Zhou J, Qu F, Barry JA, Pan JX, Wang FF, Fu ZhZh, et al. An atractylodes macrocephala koidz extract alleviates hyperandrogenism of polycystic ovarian syndrome. Int J Clin Exp Med 2016; 9: 2758-2767.
31. Dawane JS, Pandit V, Khade KS, Suryawanshi SP, Wele A, Pawar M, et al. Study the efficacy of herbal formulation Niśāmalakī in animal model of polycystic ovarian disease syndrome. Ancient Sci Life 2017; 37: 86-93.
32. Foroozandeh M, Hosseini SE. [Effects of metformin and ginger rhizome extract on the pituitary-gonad function in adult female rats with polycystic ovary syndrome]. Armaghane Danesh 2017; 22: 337-349. ( in Persian)
33. Rajan RK, Kumar SS, Balaji B. Soy isoflavones exert beneficial effects on letrozole-induced rat polycystic ovary syndrome (PCOS) model through the antiandrogenic mechanism. Pharm Biol 2017; 55: 242-251. [DOI:10.1080/13880209.2016.1258425] [PMID] [PMCID]
34. Dou L, Zheng Y, Li L, Gui X, Chen Y, Yu M, et al. The effect of cinnamon on polycystic ovary syndrome in a mouse model. Reprod Biol Endocrinol 2018; 16: 99-108. [DOI:10.1186/s12958-018-0418-y] [PMID] [PMCID]
35. Jahan S, Abid A, Khalid S, Afsar T, Ain QU, Shahee G, et al. Therapeutic potentials of quercetin in management of polycystic ovarian syndrome using letrozole induced rat model: A histological and a biochemical study. J Ovarian Res 2018; 11: 26-35. [DOI:10.1186/s13048-018-0400-5] [PMID] [PMCID]
36. Lee YH, Yang H, Lee SR, Kwon SW, Hong EJ, Lee HW. Welsh onion root (allium fistulosum) restores ovarian functions from letrozole induced-polycystic ovary syndrome. Nutrients 2018; 10: 1430-1443. [DOI:10.3390/nu10101430] [PMID] [PMCID]
37. Tahmasebi F, Movahedin M, Mazaheri Z. Antioxidant effects of calligonum extract on ovarian tissue of PCO model: An experimental study. Int J Reprod Biomed 2018; 16: 641-648. [DOI:10.29252/ijrm.16.10.641] [PMID] [PMCID]
38. Yang H, Lee SY, Lee SR, Pyun BJ, Kim HJ, Lee YH, et al. Therapeutic effect of ecklonia cava extract in letrozole-induced polycystic ovary syndrome rats. Front Pharmacol 2018; 9: 1325-1336. [DOI:10.3389/fphar.2018.01325] [PMID] [PMCID]
39. Yang H, Kim HJ, Pyun BJ, Lee HW. Licorice ethanol extract improves symptoms of polycystic ovary syndrome in letrozole-induced female rats. Integr Med Res 2018; 7: 264-270. [DOI:10.1016/j.imr.2018.05.003] [PMID] [PMCID]
40. Kakadia N, Patel P, Deshpande S, Shah G. Effect of vitex negundo L. seeds in letrozole induced polycystic ovarian syndrome. J Tradit Complement Med 2019; 9: 336-345. [DOI:10.1016/j.jtcme.2018.03.001] [PMID] [PMCID]
41. Miao M, Peng M, Zhu Z, Yan X, Wei Z, Li M. Effects of dodder total flavone on polycystic ovary syndrome rat models induced by DHEA combined HCG. Saudi J Biol Sci 2019; 26: 821-827. [DOI:10.1016/j.sjbs.2019.02.007] [PMID] [PMCID]
42. Ndeingang ECh, Deeh PBD, Watcho P, Kamanyi A. Phyllanthus muellerianus (euphorbiaceae) restores ovarian functions in letrozole-induced polycystic ovarian syndrome in rats. Evid Based Complement Alternat Med 2019; 2019: 2965821. [DOI:10.1155/2019/2965821] [PMID] [PMCID]
43. Li MF, Zhou XM, Li XL. The effect of berberine on polycystic ovary syndrome patients with insulin resistance (PCOS-IR): A meta-analysis and systematic review. Evid Based Complement Alternat Med 2018; 2018: 2532935. [DOI:10.1155/2018/2532935] [PMID] [PMCID]
44. Nyagolova PV, Mitkov MD, Orbetzova MM, Terzieva DD. Kisspeptin and galanin-like peptide (GALP) levels in women with polycystic ovary syndrome. Int J Pharmaceut Med Res 2016; 4: 7-12.
45. Binnetoglu EM, Erbag GO, Gencer M, Turkon HA, Asik ME, Gunes FA, et al. Plasma levels of nesfatin-1 in patients with polycystic ovary syndrome. Acta Medica Mediterranea 2014; 30: 201-204. [DOI:10.1530/endoabs.35.P620]
46. Baranowska B, Radzikowska M, Wasilewska-Dziubinska E, Kaplinski K, Phonowski A. Neuropeptide Y, leptin, galanin and insulin in women with polycystic ovary syndrome. Gynecol Endocrinol 1999; 13: 344-351. [DOI:10.3109/09513599909167578] [PMID]
47. Azin F, Khazali H. Neuropeptide galanin and its effects on metabolic and reproductive disturbances in female rats with estradiol valerate (EV)-induced polycystic ovary syndrome (PCOS). Neuropeptides 2020; 80: 102026. [DOI:10.1016/j.npep.2020.102026] [PMID]
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |








