Thu, Jun 11, 2026
[Archive]
Volume 23, Issue 9 (September 2025)
IJRM 2025, 23(9): 759-766 |
Back to browse issues page
Ethics code: IR.IAU.MSHD.REC.1399.045
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Delarami M, Afzali N, Hasanzadeh Mofrad M. Comparison of magnetic resonance imaging findings with and without intravenous contrast in women with pelvic endometriosis: A cross-sectional study. IJRM 2025; 23 (9) :759-766
URL: http://ijrm.ir/article-1-3492-en.html
URL: http://ijrm.ir/article-1-3492-en.html
1- Innovative Medical Research Center, MMS.C., Islamic Azad University, Mashhad, Iran.
2- Department of Radiology, MMS.C., Islamic Azad University, Mashhad, Iran. ,narges.afzali.b@gmail.com; narges.afzali@iau.ac.ir
3- Department of Obstetrics and Gynaecology, School of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran.
2- Department of Radiology, MMS.C., Islamic Azad University, Mashhad, Iran. ,
3- Department of Obstetrics and Gynaecology, School of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran.
Full-Text [PDF 874 kb]
(1156 Downloads)
| Abstract (HTML) (686 Views)
Full-Text: (139 Views)
1. Introduction
Endometriosis is the growth of endometrial tissue outside the uterine cavity, which can respond to ovarian hormonal stimulation (1). This tissue may be present in the pelvis or outside of it. The disease is commonly observed in the pelvis, ovaries, posterior cul-de-sac, uterine ligaments, pelvic cul-de-sac, and rectovaginal septum, and it is found in approximately 10% of women of reproductive age (2, 3). Infertility occurs in 30% of women with endometriosis, and up to 50% of infertile women have endometriosis (4).
Causes of infertility in this disease include adhesions in the uterus and fallopian tubes, inflammation due to the ectopic presence of endometrial tissue, increased inflammatory factors such as prostaglandins, interleukins, and tumor necrosis factors in the space around the egg and sperm, as well as hormonal changes resulting from high estradiol synthesis in peripheral tissue and decreased progesterone effect in the luteal phase of the menstrual cycle (5).
Ultrasound is the first-line imaging tool for evaluating pelvic endometriosis; however, has limitations such as field of view and operator dependency (6, 7). Laparoscopic surgery and histological confirmation of endometrial glands and/or stroma have been considered the gold standard for diagnosing the disease. Magnetic resonance imaging (MRI) is usually performed as a supplementary study in pre-surgical planning and is highly accurate in assessing endometriosis, especially deep infiltrative endometriosis (8).
There is no consensus on the role of intravenous (IV) gadolinium in the MRI protocols for diagnosing endometriosis.
This study aimed to compare the diagnostic accuracy of MRI without IV contrast injection vs. MRI with contrast injection in detecting pelvic endometriosis.
2. Materials and Methods
2.1. Study design
This cross-sectional study was conducted on 100 reproductive-aged women (15-45 yr), diagnosed with endometriosis through transvaginal ultrasound, MRI or open surgery, laparoscopy, and biopsy at gynecology clinics of 22 Bahman and Ghaem hospital, Mashhad, Iran from April 2021-July 2023.
Pelvic MRI was performed at the discretion of the gynecologist for more accurate imaging before surgery or for treatment follow-up. This study consisted of one group; however, the subpopulation analyses were done based on the age of participants. The participants were then stratified into 3 age groups: < 25 yr, 25-40 yr, and > 40 yr.
2.2. Eligibility criteria
The inclusion criteria consisted of women, aged between 15 and 45 yr, with a confirmed diagnosis of endometriosis, established either by previous pelvic ultrasound findings or through intraoperative findings at prior laparoscopy or surgery. After meeting these criteria, all eligible women underwent pelvic MRI with and without IV contrast, which was performed to allow a more detailed assessment of deep pelvic endometriosis as well as to evaluate the characteristics of endometriomas.
The exclusion criteria consisted of women with contraindications to contrast injection, such as a history of allergy to contrast agents or renal failure (with elevated creatinine level), contraindication to MRI, such as the presence of metal density in the body (e.g., implants in heart valves or cochlear implants, pacemakers, and insulin pumps), and pregnancy.
2.3. MRI protocol
All participants underwent pelvic MRI with and without IV contrast using a 1.5 Tesla Siemens MRI scanner. To improve image quality and reduce motion artifacts, intramuscular hyoscine was administered to reduce bowel peristalsis. Vaginal and rectal gel were applied locally to enhance contrast in the pelvic compartments.
The imaging protocol included the following sequences: T1-weighted (T1W), T2-weighted (T2W), T1 fat-saturated (pre- and post-contrast, and Post-contrast T1W sequences in axial, sagittal, and coronal planes following gadolinium injection (0.2 mL/kg body weight).
All images were interpreted in 2 separate sessions (pre- and post-contrast) by a single radiologist with 5 yr of experience in pelvic MRI and endometriosis. To minimize potential bias, the MRI findings with and without IV contrast were analyzed independently, without cross-referencing between the 2 modalities. MRI evaluation included assessment for: Ovarian endometriomas, and Deep infiltrating endometriosis (DIE) in the anterior and posterior pelvic compartments, particularly in the rectosigmoid colon, posterior uterine wall, uterosacral ligaments, and torus uterinus.
In cases of uncertainty during image interpretation, the radiologist re-evaluated the findings using multiplanar sequences (axial, sagittal, and coronal) and cross-checked anatomical landmarks. To ensure consistency and avoid inter-observer variability, no second-reader review was performed, and all reports were finalized by the same radiologist.
Findings from pre- and post-contrast studies were documented and compared using a standardized data collection checklist, and the results were statistically analyzed.
2.4. Sample size
Sample size was calculated using McNemar's test based on findings from Bazot et al. which reported diagnostic accuracy of 73.4% for conventional MRI and 83.5% for post-contrast MRI in detecting pelvic endometriosis (7). With a power of 90% and an alpha of 0.05, accounting for a 5% dropout rate, the sample size was estimated at 100 participants according to the following formula.
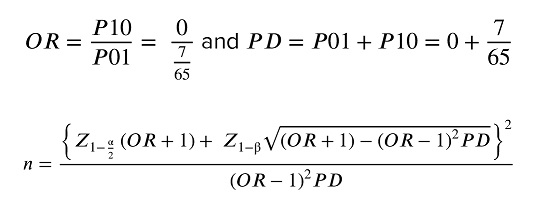
OR: odds ratio; P10/P01: discordant pairs; PD: P10+P01; Z: standard normal deviate: n: sample size; α: significance level (type I error); β: type II error (power: 1-β).
2.5. Ethical Considerations
This study was approved by the Research Council of the Faculty of Medicine, Islamic Azad University, Mashhad, Iran (Code: IR.IAU.MSHD.REC.1399.045). Written informed consent was obtained from all participants. The confidentiality of participants' personal information was strictly maintained throughout the study by the project administrator. The study procedures were in accordance with the Declaration of Helsinki.
2.6. Statistical Analysis
Statistical analyses were conducted using statistical package for the social sciences version 16.0 (SPSS Inc., Chicago, IL, USA). Descriptive statistics (mean, median, SD, range) were used for continuous variables; frequencies and percentages for categorical variables. Wilcoxon signed-rank test was applied to compare paired continuous variables (e.g., lesion depth) between pre- and post-contrast images. McNemar test was used for paired categorical data (e.g., presence/absence of DIE). Data normality was assessed using Shapiro-Wilk and Kolmogorov-Smirnov tests. A p < 0.05 was considered statistically significant.
3. Results
This study included 100 women with pelvic endometriosis, aged between 15 and 45 yr. The participants were stratified into 3 age groups: < 25 yr, 25-40 yr, and > 40 yr. The highest frequency of cases was observed in the 25-40 yr group (72%), followed by the < 25 group (16%) and the > 40 group (12%).
A history of infertility was documented in 42 participants, whereas the remaining 58 participants (58%) reported no infertility. Regarding detecting ovarian endometriomas, non-contrast MRI identified 15 cases in the < 25 group, 69 cases in the 25-40 group, and 11 cases in the > 40 group.
Post-contrast MRI yielded similar findings, with 14, 68, and 11 cases demonstrating no significant difference between pre- and post-contrast imaging (p = 0.70).
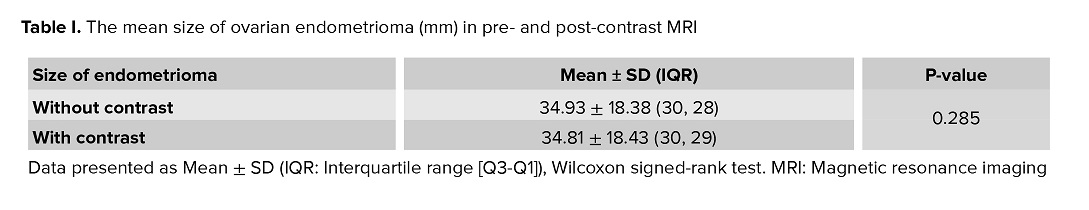
Additionally, no significant difference was noted in the mean size of ovarian endometriomas between non-contrast and post-contrast images (Table I).
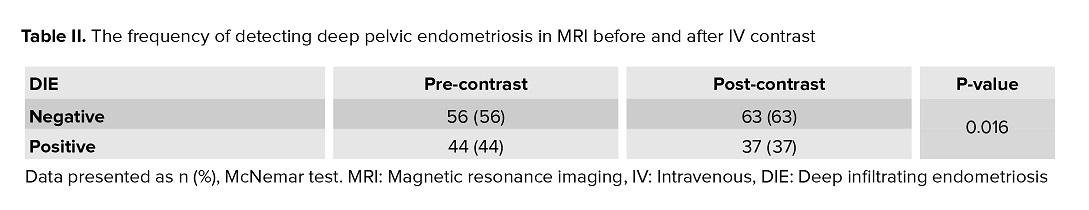
The frequency of deep pelvic endometriosis, as visualized on MRI, is summarized in table II. Comparative analysis revealed a significant increase in the detection of these lesions following contrast administration (p = 0.016) (Table II).
Although table II shows an increased number of negative findings post-contrast, this likely reflects a change in interpretation thresholds due to contrast-related masking of subtle non-enhancing lesions.
On pre-contrast images, rectal wall involvement was observed in 9% of participants, and posterior uterine wall involvement was identified in 7%, which remained constant in the post-contrast study.
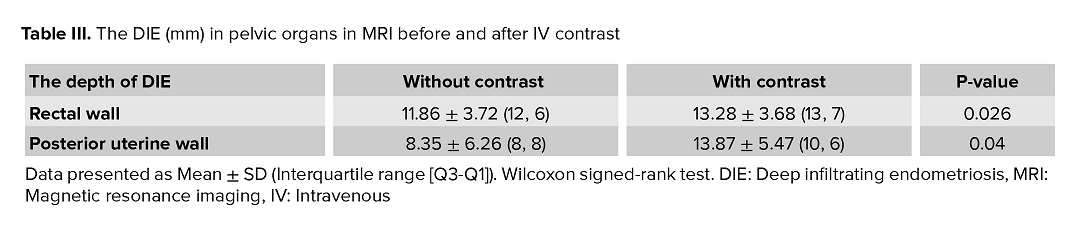
Table III provides a detailed evaluation of the depth of DIE, comparing findings between pre- and post-contrast MRI images. Regarding the depth of DIE, contrast-enhanced imaging significantly increased the detection of rectal wall involvement (p = 0.026) and posterior uterine wall involvement (p = 0.04) (Table III).
Interestingly, deep endometriosis of the torus uterus was identified in 19 pre-contrast MRI, which decreased to 12 cases on post-contrast imaging (p = 0.016). Similarly, involvement of the uterosacral ligaments was reported in 24 cases on pre-contrast images, but this decreased significantly to 15 cases with post-contrast imaging (p = 0.004).

4. Discussion
Diagnosing endometriosis and assessing the extent of pelvic involvement remain challenging. Advances in imaging, particularly transvaginal ultrasound and MRI, have improved the diagnosis of endometriomas, DIE, and adenomyosis (9, 10). The present study aimed to compare pelvic MRI with and without IV contrast in detecting endometriosis.
Our results showed no significant difference in the size or detection rate of ovarian endometriomas between pre- and post-contrast MRI. Similarly, rectal wall and posterior uterine involvement were consistently detected in both methods. In contrast, DE of the uterosacral ligaments and torus uterinus was better visualized on non-contrast MRI, suggesting that contrast may not always improve diagnostic yield.
These findings are consistent with the American College of Radiology (ACR) Appropriateness Criteria in 2024, which emphasize that the diagnostic role of IV contrast in DE remains uncertain (11). Several studies confirm that non-contrast MRI sequences (T1, T2, and DWI) provide excellent diagnostic accuracy, with contrast reserved for equivocal adnexal findings or suspected malignant mural nodules (12, 13).
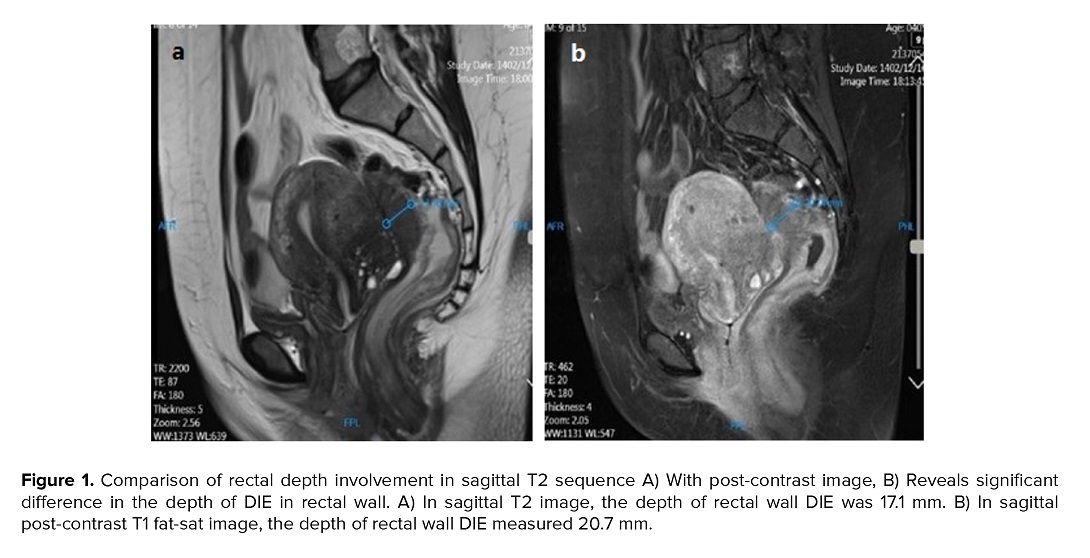
Conversely, for rectosigmoid and posterior uterine wall endometriosis, contrast-enhanced MRI highlighted greater lesion depth and posterior wall thickness (Figure 1a, b), findings aligned with a 2019 Chinese study (14). However, the number of detected lesions in the uterosacral ligaments and torus uterinus decreased significantly on post-contrast images, reinforcing the superiority of non-contrast imaging for these sites (7).
While some studies, such as a 2017 report, found no added value of IV gadolinium for rectosigmoid, vaginal, or bladder involvement (15), contrast can enhance lesion conspicuity in complex anatomical regions by highlighting neovascularized or inflamed tissue (14). This physiological basis explains why contrast may be useful in specific contexts but unnecessary in routine practice.
Optimal MRI protocol selection remains crucial. T2-weighted imaging is effective for detecting fibrotic nodules, while fat-suppressed T1-weighted sequences detect hemorrhagic lesions. Contrast may improve specificity for differentiating endometriomas from other adnexal masses (13). Some factors such as hormonal status, menstrual phase, and prior treatments influence the appearance of the lesions on MRI. Better lesion delineation is obtained in the proliferative phase of the menstrual cycle (12). Additionally, diagnostic accuracy is affected by reader expertise; inter-observer variability in DE interpretation has been documented (8). To reduce variability, our study employed a single expert radiologist. Non-contrast and contrast-enhanced MRIs were analyzed independently to minimize interpretation bias, in accordance with recommended best practices.
Taken together, these findings indicate that non-contrast pelvic MRI is sufficient in most patients, with IV contrast reserved for selected cases, particularly when evaluating lesion depth in the posterior uterine wall and rectal wall or excluding malignancy in adnexal masses. A selective rather than routine approach to gadolinium use appears most appropriate.
5. Conclusion
Based on the analysis, no significant difference was observed in the frequency of detection of ovarian endometrioma on pre- and post-contrast MRI. Regarding the size of endometrioma, no significant difference was observed in images with and without IV contrast.
The frequency of detection of DE in uterosacral ligaments and torus uterinus was higher in non-contrast images, and contrast injection reduced the likelihood of detecting endometriosis in these areas; however, the depth of the endometriosis in rectal wall and posterior uterine wall was significantly greater in post-contrast images compared to non-contrast images and IV contrast pelvic MRI can help to detect the extent of DE in these anatomic sites.
Data Availability
The data and materials of the current study are available upon reasonable request from the corresponding author.
Author Contributions
M. Hasanzadeh Mofrad conducted the experiments. N. Afzali conceived the study and wrote the manuscript. M. Delarami analyzed the data. All authors contributed to the design of the study, as well as data collection and analysis, and the writing of the manuscript. All authors read and approved the final manuscript.
Acknowledgments
The authors thank the staff and participants of this study for their important contributions. This study was conducted without external financial support. We did not use artificial intelligence in any way (translation, revision, grammar check, etc.).
Conflict of Interest
The authors declare that there is no conflict of interest.
Causes of infertility in this disease include adhesions in the uterus and fallopian tubes, inflammation due to the ectopic presence of endometrial tissue, increased inflammatory factors such as prostaglandins, interleukins, and tumor necrosis factors in the space around the egg and sperm, as well as hormonal changes resulting from high estradiol synthesis in peripheral tissue and decreased progesterone effect in the luteal phase of the menstrual cycle (5).
Ultrasound is the first-line imaging tool for evaluating pelvic endometriosis; however, has limitations such as field of view and operator dependency (6, 7). Laparoscopic surgery and histological confirmation of endometrial glands and/or stroma have been considered the gold standard for diagnosing the disease. Magnetic resonance imaging (MRI) is usually performed as a supplementary study in pre-surgical planning and is highly accurate in assessing endometriosis, especially deep infiltrative endometriosis (8).
There is no consensus on the role of intravenous (IV) gadolinium in the MRI protocols for diagnosing endometriosis.
This study aimed to compare the diagnostic accuracy of MRI without IV contrast injection vs. MRI with contrast injection in detecting pelvic endometriosis.
2. Materials and Methods
2.1. Study design
This cross-sectional study was conducted on 100 reproductive-aged women (15-45 yr), diagnosed with endometriosis through transvaginal ultrasound, MRI or open surgery, laparoscopy, and biopsy at gynecology clinics of 22 Bahman and Ghaem hospital, Mashhad, Iran from April 2021-July 2023.
Pelvic MRI was performed at the discretion of the gynecologist for more accurate imaging before surgery or for treatment follow-up. This study consisted of one group; however, the subpopulation analyses were done based on the age of participants. The participants were then stratified into 3 age groups: < 25 yr, 25-40 yr, and > 40 yr.
2.2. Eligibility criteria
The inclusion criteria consisted of women, aged between 15 and 45 yr, with a confirmed diagnosis of endometriosis, established either by previous pelvic ultrasound findings or through intraoperative findings at prior laparoscopy or surgery. After meeting these criteria, all eligible women underwent pelvic MRI with and without IV contrast, which was performed to allow a more detailed assessment of deep pelvic endometriosis as well as to evaluate the characteristics of endometriomas.
The exclusion criteria consisted of women with contraindications to contrast injection, such as a history of allergy to contrast agents or renal failure (with elevated creatinine level), contraindication to MRI, such as the presence of metal density in the body (e.g., implants in heart valves or cochlear implants, pacemakers, and insulin pumps), and pregnancy.
2.3. MRI protocol
All participants underwent pelvic MRI with and without IV contrast using a 1.5 Tesla Siemens MRI scanner. To improve image quality and reduce motion artifacts, intramuscular hyoscine was administered to reduce bowel peristalsis. Vaginal and rectal gel were applied locally to enhance contrast in the pelvic compartments.
The imaging protocol included the following sequences: T1-weighted (T1W), T2-weighted (T2W), T1 fat-saturated (pre- and post-contrast, and Post-contrast T1W sequences in axial, sagittal, and coronal planes following gadolinium injection (0.2 mL/kg body weight).
All images were interpreted in 2 separate sessions (pre- and post-contrast) by a single radiologist with 5 yr of experience in pelvic MRI and endometriosis. To minimize potential bias, the MRI findings with and without IV contrast were analyzed independently, without cross-referencing between the 2 modalities. MRI evaluation included assessment for: Ovarian endometriomas, and Deep infiltrating endometriosis (DIE) in the anterior and posterior pelvic compartments, particularly in the rectosigmoid colon, posterior uterine wall, uterosacral ligaments, and torus uterinus.
In cases of uncertainty during image interpretation, the radiologist re-evaluated the findings using multiplanar sequences (axial, sagittal, and coronal) and cross-checked anatomical landmarks. To ensure consistency and avoid inter-observer variability, no second-reader review was performed, and all reports were finalized by the same radiologist.
Findings from pre- and post-contrast studies were documented and compared using a standardized data collection checklist, and the results were statistically analyzed.
2.4. Sample size
Sample size was calculated using McNemar's test based on findings from Bazot et al. which reported diagnostic accuracy of 73.4% for conventional MRI and 83.5% for post-contrast MRI in detecting pelvic endometriosis (7). With a power of 90% and an alpha of 0.05, accounting for a 5% dropout rate, the sample size was estimated at 100 participants according to the following formula.
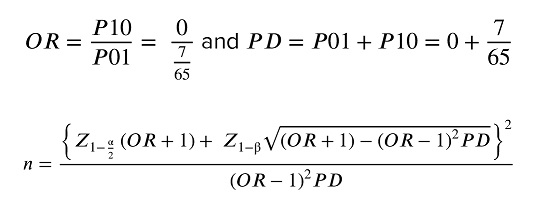
OR: odds ratio; P10/P01: discordant pairs; PD: P10+P01; Z: standard normal deviate: n: sample size; α: significance level (type I error); β: type II error (power: 1-β).
2.5. Ethical Considerations
This study was approved by the Research Council of the Faculty of Medicine, Islamic Azad University, Mashhad, Iran (Code: IR.IAU.MSHD.REC.1399.045). Written informed consent was obtained from all participants. The confidentiality of participants' personal information was strictly maintained throughout the study by the project administrator. The study procedures were in accordance with the Declaration of Helsinki.
2.6. Statistical Analysis
Statistical analyses were conducted using statistical package for the social sciences version 16.0 (SPSS Inc., Chicago, IL, USA). Descriptive statistics (mean, median, SD, range) were used for continuous variables; frequencies and percentages for categorical variables. Wilcoxon signed-rank test was applied to compare paired continuous variables (e.g., lesion depth) between pre- and post-contrast images. McNemar test was used for paired categorical data (e.g., presence/absence of DIE). Data normality was assessed using Shapiro-Wilk and Kolmogorov-Smirnov tests. A p < 0.05 was considered statistically significant.
3. Results
This study included 100 women with pelvic endometriosis, aged between 15 and 45 yr. The participants were stratified into 3 age groups: < 25 yr, 25-40 yr, and > 40 yr. The highest frequency of cases was observed in the 25-40 yr group (72%), followed by the < 25 group (16%) and the > 40 group (12%).
A history of infertility was documented in 42 participants, whereas the remaining 58 participants (58%) reported no infertility. Regarding detecting ovarian endometriomas, non-contrast MRI identified 15 cases in the < 25 group, 69 cases in the 25-40 group, and 11 cases in the > 40 group.
Post-contrast MRI yielded similar findings, with 14, 68, and 11 cases demonstrating no significant difference between pre- and post-contrast imaging (p = 0.70).
Additionally, no significant difference was noted in the mean size of ovarian endometriomas between non-contrast and post-contrast images (Table I).
The frequency of deep pelvic endometriosis, as visualized on MRI, is summarized in table II. Comparative analysis revealed a significant increase in the detection of these lesions following contrast administration (p = 0.016) (Table II).
Although table II shows an increased number of negative findings post-contrast, this likely reflects a change in interpretation thresholds due to contrast-related masking of subtle non-enhancing lesions.
On pre-contrast images, rectal wall involvement was observed in 9% of participants, and posterior uterine wall involvement was identified in 7%, which remained constant in the post-contrast study.
Table III provides a detailed evaluation of the depth of DIE, comparing findings between pre- and post-contrast MRI images. Regarding the depth of DIE, contrast-enhanced imaging significantly increased the detection of rectal wall involvement (p = 0.026) and posterior uterine wall involvement (p = 0.04) (Table III).
Interestingly, deep endometriosis of the torus uterus was identified in 19 pre-contrast MRI, which decreased to 12 cases on post-contrast imaging (p = 0.016). Similarly, involvement of the uterosacral ligaments was reported in 24 cases on pre-contrast images, but this decreased significantly to 15 cases with post-contrast imaging (p = 0.004).



4. Discussion
Diagnosing endometriosis and assessing the extent of pelvic involvement remain challenging. Advances in imaging, particularly transvaginal ultrasound and MRI, have improved the diagnosis of endometriomas, DIE, and adenomyosis (9, 10). The present study aimed to compare pelvic MRI with and without IV contrast in detecting endometriosis.
Our results showed no significant difference in the size or detection rate of ovarian endometriomas between pre- and post-contrast MRI. Similarly, rectal wall and posterior uterine involvement were consistently detected in both methods. In contrast, DE of the uterosacral ligaments and torus uterinus was better visualized on non-contrast MRI, suggesting that contrast may not always improve diagnostic yield.
These findings are consistent with the American College of Radiology (ACR) Appropriateness Criteria in 2024, which emphasize that the diagnostic role of IV contrast in DE remains uncertain (11). Several studies confirm that non-contrast MRI sequences (T1, T2, and DWI) provide excellent diagnostic accuracy, with contrast reserved for equivocal adnexal findings or suspected malignant mural nodules (12, 13).
Conversely, for rectosigmoid and posterior uterine wall endometriosis, contrast-enhanced MRI highlighted greater lesion depth and posterior wall thickness (Figure 1a, b), findings aligned with a 2019 Chinese study (14). However, the number of detected lesions in the uterosacral ligaments and torus uterinus decreased significantly on post-contrast images, reinforcing the superiority of non-contrast imaging for these sites (7).
While some studies, such as a 2017 report, found no added value of IV gadolinium for rectosigmoid, vaginal, or bladder involvement (15), contrast can enhance lesion conspicuity in complex anatomical regions by highlighting neovascularized or inflamed tissue (14). This physiological basis explains why contrast may be useful in specific contexts but unnecessary in routine practice.
Optimal MRI protocol selection remains crucial. T2-weighted imaging is effective for detecting fibrotic nodules, while fat-suppressed T1-weighted sequences detect hemorrhagic lesions. Contrast may improve specificity for differentiating endometriomas from other adnexal masses (13). Some factors such as hormonal status, menstrual phase, and prior treatments influence the appearance of the lesions on MRI. Better lesion delineation is obtained in the proliferative phase of the menstrual cycle (12). Additionally, diagnostic accuracy is affected by reader expertise; inter-observer variability in DE interpretation has been documented (8). To reduce variability, our study employed a single expert radiologist. Non-contrast and contrast-enhanced MRIs were analyzed independently to minimize interpretation bias, in accordance with recommended best practices.
Taken together, these findings indicate that non-contrast pelvic MRI is sufficient in most patients, with IV contrast reserved for selected cases, particularly when evaluating lesion depth in the posterior uterine wall and rectal wall or excluding malignancy in adnexal masses. A selective rather than routine approach to gadolinium use appears most appropriate.

5. Conclusion
Based on the analysis, no significant difference was observed in the frequency of detection of ovarian endometrioma on pre- and post-contrast MRI. Regarding the size of endometrioma, no significant difference was observed in images with and without IV contrast.
The frequency of detection of DE in uterosacral ligaments and torus uterinus was higher in non-contrast images, and contrast injection reduced the likelihood of detecting endometriosis in these areas; however, the depth of the endometriosis in rectal wall and posterior uterine wall was significantly greater in post-contrast images compared to non-contrast images and IV contrast pelvic MRI can help to detect the extent of DE in these anatomic sites.
Data Availability
The data and materials of the current study are available upon reasonable request from the corresponding author.
Author Contributions
M. Hasanzadeh Mofrad conducted the experiments. N. Afzali conceived the study and wrote the manuscript. M. Delarami analyzed the data. All authors contributed to the design of the study, as well as data collection and analysis, and the writing of the manuscript. All authors read and approved the final manuscript.
Acknowledgments
The authors thank the staff and participants of this study for their important contributions. This study was conducted without external financial support. We did not use artificial intelligence in any way (translation, revision, grammar check, etc.).
Conflict of Interest
The authors declare that there is no conflict of interest.
Type of Study: Original Article |
Subject:
Fertility & Infertility
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |







