Volume 24, Issue 2 (February 2026)
IJRM 2026, 24(2): 0-0 |
Back to browse issues page
Ethics code: IR.TUMS.IKHC.REC.1403.124
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Khazardoust S, Zamanpour Z, Aliasgharpoor M, Shafaat M A, Hamidi Madani Z, Ghalandari M. Evaluating the diagnostic efficacy of cervical length and angles in predicting delivery mode: A cross-sectional study. IJRM 2026; 24 (2)
URL: http://ijrm.ir/article-1-3581-en.html
URL: http://ijrm.ir/article-1-3581-en.html
Soghra Khazardoust1 

 , Zeinab Zamanpour2
, Zeinab Zamanpour2 

 , Maryam Aliasgharpoor3
, Maryam Aliasgharpoor3 

 , Mohammad Ali Shafaat4
, Mohammad Ali Shafaat4 

 , Zahra Hamidi Madani *5
, Zahra Hamidi Madani *5 

 , Maryam Ghalandari6
, Maryam Ghalandari6 




 , Zeinab Zamanpour2
, Zeinab Zamanpour2 

 , Maryam Aliasgharpoor3
, Maryam Aliasgharpoor3 

 , Mohammad Ali Shafaat4
, Mohammad Ali Shafaat4 

 , Zahra Hamidi Madani *5
, Zahra Hamidi Madani *5 

 , Maryam Ghalandari6
, Maryam Ghalandari6 


1- Department of Obstetrics and Gynecology, Maternal, Fetal and Neonatal Research Center, Family Health Research Institute, Imam Khomeini Hospital Complex, School of Medicine, Tehran University of Medical Sciences, Tehran, Iran.
2- Department of Obstetrics and Gynecology, School of Medicine, Jundishapour University of Medical Sciences, Ahvaz, Iran.
3- Vali-E-Asr Reproductive Health Research Center, Family Health Research Institute, Imam Khomeini Hospital Complex, Tehran University of Medical Sciences, Tehran, Iran.
4- Department of Obstetrics and Gynecology, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
5- Department of Obstetrics and Gynecology, Reproductive Health Research Center, School of Medicine, Guilan University of Medical Sciences, Rasht, Iran. ,Zahra_hamidi@gums.ac.ir; Tannaz.hamid1369@gmail.com
6- Vice-Chancellorship of Research and Technology, Guilan University of Medical Sciences, Rasht, Iran.
2- Department of Obstetrics and Gynecology, School of Medicine, Jundishapour University of Medical Sciences, Ahvaz, Iran.
3- Vali-E-Asr Reproductive Health Research Center, Family Health Research Institute, Imam Khomeini Hospital Complex, Tehran University of Medical Sciences, Tehran, Iran.
4- Department of Obstetrics and Gynecology, Shahid Beheshti University of Medical Sciences, Tehran, Iran.
5- Department of Obstetrics and Gynecology, Reproductive Health Research Center, School of Medicine, Guilan University of Medical Sciences, Rasht, Iran. ,
6- Vice-Chancellorship of Research and Technology, Guilan University of Medical Sciences, Rasht, Iran.
Abstract: (23 Views)
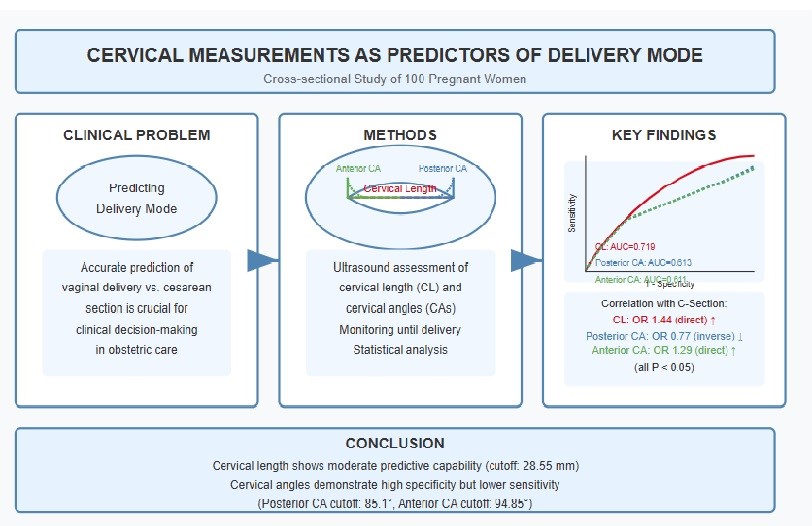
Background: Predicting delivery mode is crucial to obstetric care and influences clinical decision-making and management strategies.
Objective: This study aimed to evaluate the diagnostic efficacy of cervical length (CL) and cervical angles (CAs) measurements as predictors of delivery mode.
Materials and Methods: This cross-sectional study was conducted on 100 pregnant women who underwent ultrasound assessments to measure CL and CAs. Participants were monitored until labor induction, with delivery mode categorized as successful vaginal deliveries or cesarean sections. Statistical analyses were performed to evaluate the diagnostic value of cervical measurements in predicting these outcomes.
Results: The results demonstrate significant correlations between CL and both posterior and anterior CAs with the likelihood of cesarean sections, yielding odds ratios of 1.59, 0.68, and 1.48, respectively (p < 0.05). Diagnostic accuracy assessments indicated that the CL cutoff of 28.55 mm achieved an area under the curve of 0.801; posterior and anterior CAs, with cutoffs of 102.15° and 85.15°, respectively, produced area under the curve of 0.743 and 0.745.
Conclusion: The findings indicated that CL and the anterior CA exhibit a direct significant correlation, whereas the posterior CA showed a significant reverse correlation with the occurrence of cesarean section. The diagnostic accuracy metrics reveal that CL possesses moderate predictive capability for labor outcomes. The posterior demonstrated high sensitivity, in contrast, anterior CA had high specificity but lower sensitivity levels. The small sample size and possible measurement inaccuracies may limit the reliability of our findings, highlighting the need for larger studies with standardized techniques to validate these results.
Objective: This study aimed to evaluate the diagnostic efficacy of cervical length (CL) and cervical angles (CAs) measurements as predictors of delivery mode.
Materials and Methods: This cross-sectional study was conducted on 100 pregnant women who underwent ultrasound assessments to measure CL and CAs. Participants were monitored until labor induction, with delivery mode categorized as successful vaginal deliveries or cesarean sections. Statistical analyses were performed to evaluate the diagnostic value of cervical measurements in predicting these outcomes.
Results: The results demonstrate significant correlations between CL and both posterior and anterior CAs with the likelihood of cesarean sections, yielding odds ratios of 1.59, 0.68, and 1.48, respectively (p < 0.05). Diagnostic accuracy assessments indicated that the CL cutoff of 28.55 mm achieved an area under the curve of 0.801; posterior and anterior CAs, with cutoffs of 102.15° and 85.15°, respectively, produced area under the curve of 0.743 and 0.745.
Conclusion: The findings indicated that CL and the anterior CA exhibit a direct significant correlation, whereas the posterior CA showed a significant reverse correlation with the occurrence of cesarean section. The diagnostic accuracy metrics reveal that CL possesses moderate predictive capability for labor outcomes. The posterior demonstrated high sensitivity, in contrast, anterior CA had high specificity but lower sensitivity levels. The small sample size and possible measurement inaccuracies may limit the reliability of our findings, highlighting the need for larger studies with standardized techniques to validate these results.
Type of Study: Original Article |
Subject:
Reproductive Physiology
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |