Sat, May 23, 2026
[Archive]
Volume 23, Issue 7 (July 2025)
IJRM 2025, 23(7): 533-544 |
Back to browse issues page
Ethics code: R.ARAKMU.REC.1403.019
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Soltani M, Shojafar E, Ghafarizadeh A A, Moslemi A, Jalali Mashayekhi F, Baazm M. Comparison of the effects of platelet-rich plasma and nanocurcumin on the sperm quality parameters in frozen-thawed semen of men with asthenoteratozoospermia: A lab trial study. IJRM 2025; 23 (7) :533-544
URL: http://ijrm.ir/article-1-3613-en.html
URL: http://ijrm.ir/article-1-3613-en.html
Mahsa Soltani1 

 , Elham Shojafar2
, Elham Shojafar2 

 , Ali Asghar Ghafarizadeh2
, Ali Asghar Ghafarizadeh2 

 , Azam Moslemi3
, Azam Moslemi3 

 , Farideh Jalali Mashayekhi4
, Farideh Jalali Mashayekhi4 

 , Maryam Baazm *5
, Maryam Baazm *5 




 , Elham Shojafar2
, Elham Shojafar2 

 , Ali Asghar Ghafarizadeh2
, Ali Asghar Ghafarizadeh2 

 , Azam Moslemi3
, Azam Moslemi3 

 , Farideh Jalali Mashayekhi4
, Farideh Jalali Mashayekhi4 

 , Maryam Baazm *5
, Maryam Baazm *5 


1- Students Research Committee, Arak University of Medical Sciences, Arak, Iran.
2- Rastak Infertility Treatment Center, Sina Hospital, Arak, Iran.
3- Department of Biostatistics, School of Medicine, Arak University of Medical Sciences, Arak, Iran.
4- Department of Genetics and Biochemistry, School of Medicine, Arak University of Medical Sciences, Arak, Iran.
5- Department of Anatomy, School of Medicine, Arak University of Medical Sciences, Arak, Iran. & Molecular and Medicine Research Center, School of Medicine, Arak University of Medical Sciences, Arak, Iran. ,dr.baazm@arakmu.ac.ir
2- Rastak Infertility Treatment Center, Sina Hospital, Arak, Iran.
3- Department of Biostatistics, School of Medicine, Arak University of Medical Sciences, Arak, Iran.
4- Department of Genetics and Biochemistry, School of Medicine, Arak University of Medical Sciences, Arak, Iran.
5- Department of Anatomy, School of Medicine, Arak University of Medical Sciences, Arak, Iran. & Molecular and Medicine Research Center, School of Medicine, Arak University of Medical Sciences, Arak, Iran. ,
Abstract: (889 Views)
Background: Cryopreservation of sperm can adversely affect sperm quality, particularly in individuals with asthenoteratozoospermia. Various substances are added to the cryopreservation medium to prevent cellular damage.
Objective: This study aimed to evaluate the effects of platelet-rich plasma (PRP) and nanocurcumin (nCur) on sperm parameters, DNA fragmentation, and oxidative stress levels in cryopreserved semen.
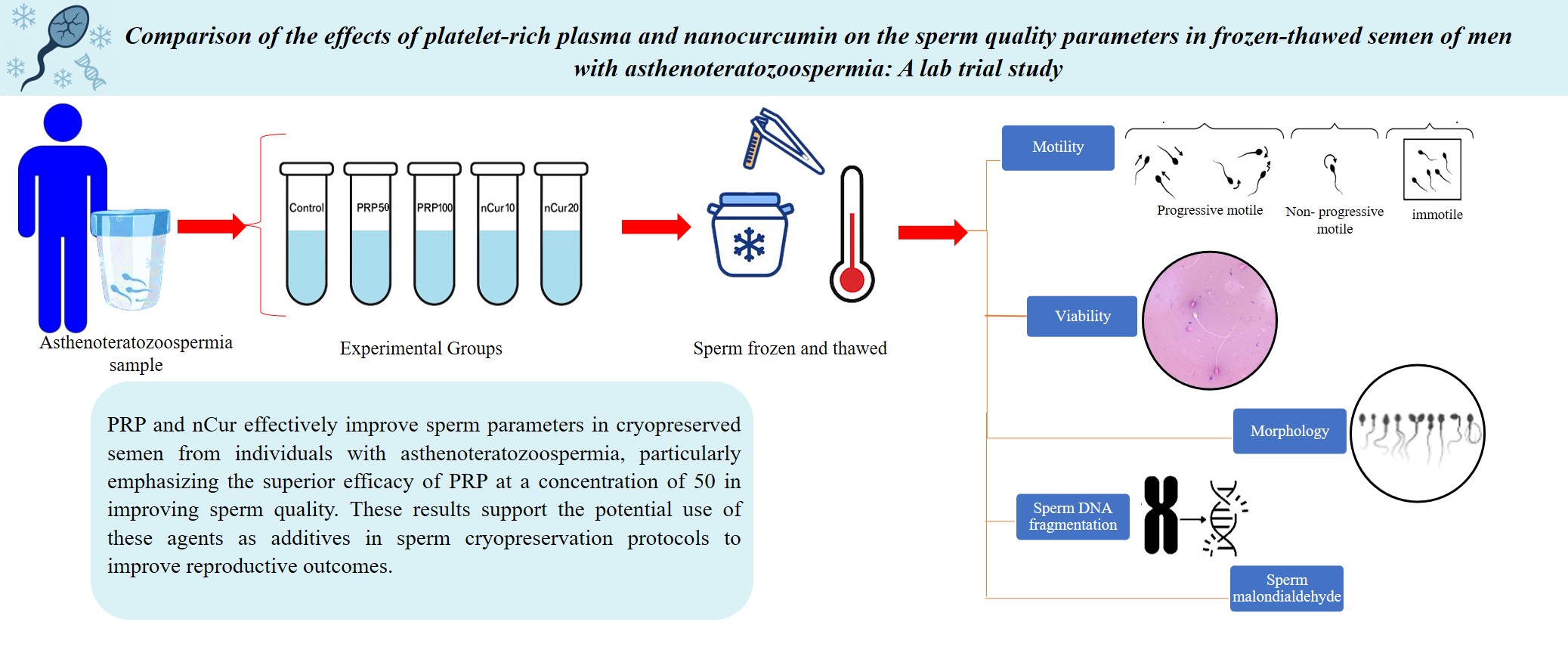
Materials and Methods: In this lab trial study, semen samples of 20 men with asthenoteratozoospermia who referred to Rastak and Ghavamzadeh Infertility Centers, Arak, Iran from June-August 2024 were collected. Each sample was divided into 5 groups: control (no treatment), PRP50, PRP100, nCur10, and nCur20. The control samples underwent freezing without additives. Post-thawing assessments included sperm motility, viability, DNA fragmentation index, and malondialdehyde levels to evaluate oxidative stress.
Results: Treatment with PRP50 (p < 0.001) and nCur20 (p = 0.001) significantly increased sperm motility compared to the control group. All treatment groups showed a significant increase in viable sperm following freezing (p < 0.001), with PRP50 demonstrating the most pronounced effects (p < 0.001). While no improvements in sperm morphology were observed after freezing, PRP and nCur significantly reduced DNA fragmentation index after freezing (p < 0.001), with PRP50 being the most effective (p < 0.001). Additionally, both PRP and nCur significantly decreased malondialdehyde levels compared to the control group (p < 0.001).
Conclusion: PRP and nCur effectively improve sperm parameters in cryopreserved semen from individuals with asthenoteratozoospermia, particularly emphasizing the superior efficacy of PRP at a concentration of 50 in improving sperm quality. These results support the potential use of these agents as additives in sperm cryopreservation protocols to improve reproductive outcomes.
Materials and Methods: In this lab trial study, semen samples of 20 men with asthenoteratozoospermia who referred to Rastak and Ghavamzadeh Infertility Centers, Arak, Iran from June-August 2024 were collected. Each sample was divided into 5 groups: control (no treatment), PRP50, PRP100, nCur10, and nCur20. The control samples underwent freezing without additives. Post-thawing assessments included sperm motility, viability, DNA fragmentation index, and malondialdehyde levels to evaluate oxidative stress.
Results: Treatment with PRP50 (p < 0.001) and nCur20 (p = 0.001) significantly increased sperm motility compared to the control group. All treatment groups showed a significant increase in viable sperm following freezing (p < 0.001), with PRP50 demonstrating the most pronounced effects (p < 0.001). While no improvements in sperm morphology were observed after freezing, PRP and nCur significantly reduced DNA fragmentation index after freezing (p < 0.001), with PRP50 being the most effective (p < 0.001). Additionally, both PRP and nCur significantly decreased malondialdehyde levels compared to the control group (p < 0.001).
Conclusion: PRP and nCur effectively improve sperm parameters in cryopreserved semen from individuals with asthenoteratozoospermia, particularly emphasizing the superior efficacy of PRP at a concentration of 50 in improving sperm quality. These results support the potential use of these agents as additives in sperm cryopreservation protocols to improve reproductive outcomes.
Keywords: Cryopreservation, Spermatozoa, Asthenoteratozoospermia, Platelet-rich plasma, Nanocurcumin.
Type of Study: Original Article |
Subject:
Reproductive Andrology
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |